Does your child have asthma? Here's how to manage it, as shared by doctors from the Respiratory Medicine service at KK Women's and Children's Hospital (KKH).
Children with asthma have air passages that are hyper-responsive (sensitive) to triggers compared to other children. Asthma may present as recurrent episodes of wheezing, breathlessness, chest tightness or coughing.
The severity of asthma differs in each child and can change with the course of time.
Up to half of the children with asthma are likely to be attack-free in their teens, while the remaining are likely to have milder and less frequent attacks.
Only five percent of children continue to have asthma in adulthood.
Here are tips on how your child can better manage asthma, with expertise from the
Respiratory Medicine service at KK Women's and Children's Hospital (KKH), a member of the
SingHealth group.
Tips to manage asthma in children
Asthma is a chronic inflammatory disease of the lower airways of the lungs. It is very common worldwide. In Singapore, about one in five children has asthma.
1. Avoid triggers that cause asthma attacks
Asthma results from sensitive airways that react to triggers. These triggers may differ from person to person. Avoidance of triggers is important. Some common triggers include:
Infections, including the common cold and flu.
Environmental allergens like house dust mites, animal dander, pollen, indoor mould.
Weather changes due to change in temperature or humidity.
Air pollution e.g. from cigarette smoke, haze.
2. Take asthma medications as prescribed by your doctor
There are two main types of asthma medications:
Controllers/preventers: These work slowly to control the chronic inflammation, making airways less sensitive to triggers. These medicines need to be used daily if prescribed by the doctor and should only be stopped when advised by the doctor. The period of treatment for each child prescribed with controllers/preventer medicines can range from many months to years, depending on the response and control of the child's asthma.
Relievers: These work rapidly to open the airways, providing quick relief of asthma symptoms. They should only be used when needed.
All children with asthma will be prescribed with a reliever medicine for use during asthma attacks. Some children whose asthma is not well controlled may need to use a controller/preventer medicine daily.
The doctor will be able to assess and advise if your child needs to use a controller/preventer medicine daily.
3. Other ways to help manage your child's asthma
Keep your child away from smokers and smoke-filled environments.
Avoid giving your child cold drinks and citrus fruits when he/she is unwell.
Get your child to rest and avoid exercise during and soon after an asthma attack.
When to consult a doctor for an asthma attack
Consult your doctor if during an asthma attack, your child:
Remains breathless despite reliever medicines following the asthma action plan by the doctor
Is unable to feed or take fluids well
Is unable to speak in complete sentences
Is drowsy, unresponsive and lethargic, or irritable and difficult to calm.
Always remember to bring your child's inhaler, spacer and action plan every time he/she visits the clinic or hospital.
What is an asthma action plan? An asthma action plan is a personalised written list of instructions that provides instructions for you to follow at home to help manage your child's asthma. It includes instructions on: What medicines your child should use at home each day What warning symptoms to watch for (which suggest that asthma is getting worse) What other medicines to give your child if the symptoms get worse When to get help or call for an ambulance
You, your child, and your doctor will work together to develop the asthma action plan. This can be useful in clarifying the medication regimen, identifying declines in asthma control, guiding treatment adjustments in response to changes in symptoms and guidance in the event your child suffers a severe asthma attack.
|
What happens during an asthma attack?
Exposure to triggers result in inflammation of the airways. The airways become narrowed and clogged with mucus. Inflammation may still be ongoing even if you do not observe any signs or symptoms.
How to use an inhaler with a spacer with mouthpiece/facemask
All metered-dose inhalers (MDIs) should be used together with a spacer as children may not be able to coordinate the inhalation process properly.
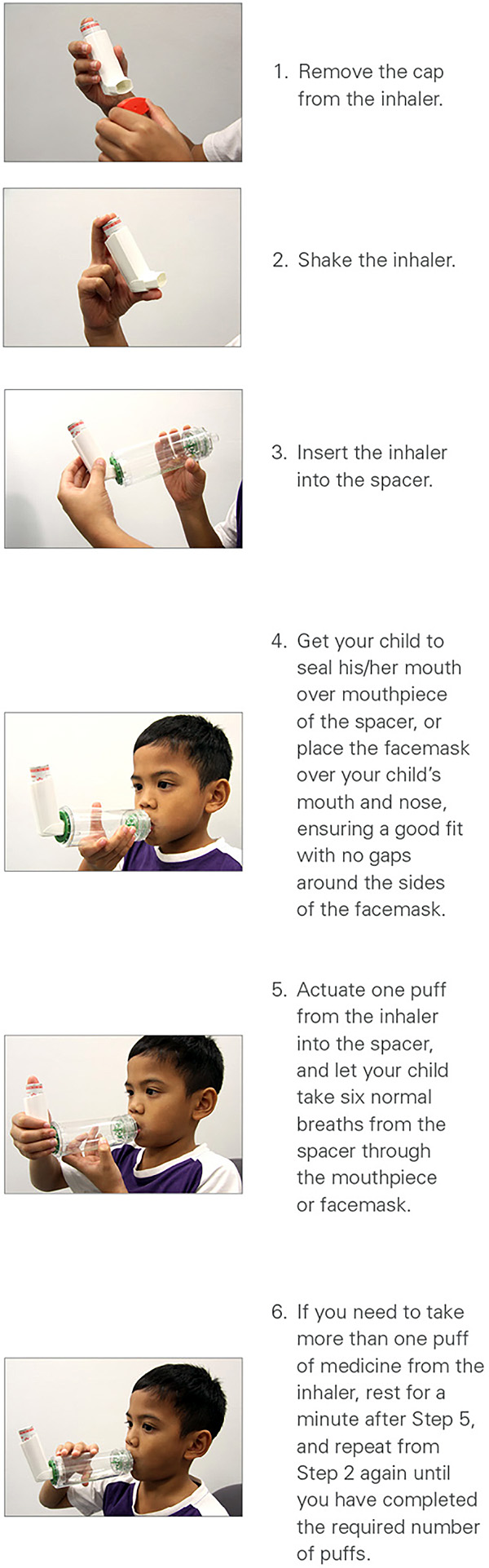
How to care for the spacer and inhaler
Clean your spacer once a week.
Soak the spacer completely in mild soapy water made by adding two to three drops of dishwashing liquid into a container of water. Do not use a scrub to clean the spacer. Do not rinse the spacer again after removing it from the soapy water.
Allow the spacer to drip dry. Do not use tissue paper or cloth to dry the spacer after washing it.
Following the steps above help to reduce the static charge in the spacer and allow for better delivery of the medicine from the inhaler to the lungs.
If you need to use the spacer urgently before it is dry after washing, prime the spacer by actuating ten puffs of reliever medication into the spacer after drying it.
Wash the plastic holder of the inhaler once a week under warm running water and air dry the plastic holder thoroughly before putting the inhaler back into it for use.
Ref: G25 (ed)
Related articles:
How to Survive an Asthma Attack if Caught Without an Inhaler
Common Asthma Triggers at Home
Can Children Outgrow Asthma?
Children's Asthma: 5 FAQs, Answered!
