Intraoperative Radiotherapy represents a significant development in reducing the treatment burden of patients undergoing treatment for early breast cancers.
Women diagnosed with early breast cancers may face a lengthy treatment with a plethora of treatment modalities. Often, the very first choice they make is in deciding the type of surgery to remove the cancer: mastectomy where the entire involved breast is removed or a more limited surgery where the tumour alone is cleanly removed with clear margins, i.e. breastconserving surgery (BCS). It is also at this time when patients often first learn of the need for post-operative radiotherapy (RT).
Without adjuvant radiotherapy, about 1 in 4 patients will recur in the breast. Long-term studies have shown that radiotherapy more than halves this risk and improves patients’ survival. As such, RT is nearly always indicated after BCS.
However, despite the many benefits of breast-conserving therapy over mastectomy in terms of preservation of body image and psychosexual health at equivalent rates of disease control, the additional 4 to 6 weeks course of radiotherapy imposes significant financial and logistical challenge to many patients.
Furthermore, adjuvant radiation to the whole breast imparts not only shortterm toxicity such as dermatitis but also low, but not negligible risks of longterm side effects to the heart, lungs and chest wall.
Accumulating data suggests that it is not always necessary to irradiate the entire breast. It has been shown that the great majority of local recurrences occur in close proximity to the index lesion. It is here that the greatest true recurrence risks lies and where adjuvant RT exerts most of its curative effects.
In contrast, adjuvant radiotherapy does not appear to reduce the incidence of non-index quadrants cancer occurrence which, incidentally, develops at a similar rate to new cancers in the opposite breast suggesting that some, if not all, of them are not related to the primary cancer.
Therefore, radiotherapy to the limited volume of highest risks around the tumour cavity may be sufficient to provide most of the disease control at minimum risks of side effects. This understanding gave rise to the concept of Accelerated Partial Breast Irradiation (APBI).
ACCELERATED PARTIAL BREAST IRRADIATION (APBI)
In APBI, the volume of breast irradiated is reduced from whole breast radiation. This reduces the amount of sensitive normal tissue irradiated and helps to reduce both short- and long-term side effects. Because of this targeted delivery of radiation to only the at-risk tissue, radiation can be given over a shorter treatment course.
Depending on the techniques of APBI used, a normal conventional course of RT that used to last 4 to 6 weeks can be reduced to 1 week or as short as a single fraction. This drastically reduces the patient’s treatment burden.
Intraoperative Radiotherapy (IORT)
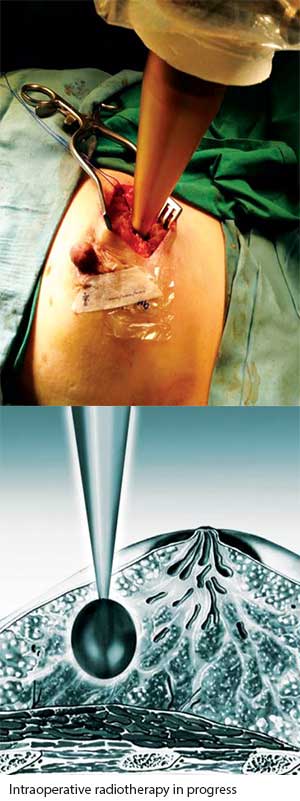 One method of APBI that has come to the forefront is the Intraoperative Radiotherapy (IORT). Since its introduction to National Cancer Centre Singapore (NCCS) 3 years ago, IORT has been the workhorse for our partial breast irradiation programme.
One method of APBI that has come to the forefront is the Intraoperative Radiotherapy (IORT). Since its introduction to National Cancer Centre Singapore (NCCS) 3 years ago, IORT has been the workhorse for our partial breast irradiation programme.
In this programme, patients are carefully selected to include only those patients in whom the risks of regional and distant metastases are low. In addition, candidates for IORT must fulfill other technical and pathological considerations including having clear margins at excision and features suggesting a low likelihood of extensive, multifocal disease. Thus, patients treated with IORT at NCCS are often the postmenopausal patients older than 50 years old with early-stage, node-negative breast cancers expressing hormone receptors.
How it is done
For patients planned for IORT, they first undergo breast conservation surgery in the usual fashion. Sentinel lymph node biopsy (SLNB) will be performed and frozen section assessment of the lymph node done while the patient is still under general anaesthesia.
Once the result shows no cancer in the SLNB, a specialised applicator is emplaced in the open excision cavity to irradiate the cavity wall and surrounding breast. In the following 30 to 40 minutes, the radiation dose that used to take 6 weeks of daily treatment to deliver will be given in one session whilst the patients remain blissfully unaware under anaesthesia.
The success of IORT is predicated on the careful selection of patients. However, certain features of high-risk disease such as the presence of extensive intraductal components (ductal carcinoma in-situ), lymphovascular invasion, positive excision margins, or false negative sentinel lymph nodes can only be determined after the operation and IORT has been performed.
In such cases, further surgery may be indicated to complete treatment and the remaining untreated breast would need further external radiotherapy. This ‘topup’ radiation typically lasts 3 weeks. The typical ‘boost’ dose given to the tumour bed in a conventional course of RT is omitted as IORT is considered equivalent.
SUMMARY
In summary, IORT represents a significant development in reducing the treatment burden of patients undergoing treatment for early breast cancers. Not only is time spent on treatment vastly reduced from 4 to 6 weeks to a single intraoperative fraction, the side effects often seen in patients undergoing conventional whole breast RT is largely avoided.
As such, IORT should be considered in all suitable patients undergoing breast conservation therapy for early breast cancers. Certainly, no woman should have to resort to choosing mastectomy as the Hobson’s choice to avoid the burden of a lengthy course of adjuvant radiotherapy.
The field of APBI has been bolstered in recent years with encouraging reports of the outcomes of several scientific studies conducted. In the randomised control trial (TARGIT-A) examining the use of conventional whole breast radiotherapy versus the use of IORT and external beam radiation when indicated, patients undergoing IORT had non-inferior local control rates and survivals.
The 5-year local failure rates among patients treated with TARGIT in the same setting as their primary surgery is a reassuring 2.1% at 5 years. Wound-related complications are the same between arms and Grade 3/4 skin toxicity is lower in the IORT arm (0.2%).
It was further observed that while breast cancer mortality is similar (2.6% vs 1.9%, p=0.56, NS); nonbreast- cancer mortality is higher in patients who received whole breast radiotherapy (1.4% vs 3.5%, p=0.0086, significant).
In NCCS, we are conducting further studies to explore if IORT can be safely delivered as an alternative to whole breast RT along with standard adjuvant systemic treatment for patients with moderate disease. We are also exploring the use of IORT in patients with pure ductal carcinoma in situ, an increasingly common diagnosis as more women undergo mammographic screening.
GPs can call for appointments through the GP Appointment Hotlines:
63214402 (SGH)
64368288 (NCCS)
62944050 (KKH)
By: Dr Wong Fuh Yong, Senior Consultant, Division of Radiation Oncology, National Cancer Centre Singapore
Dr Wong Fuh Yong is a Senior Consultant with the Division of Radiation Oncology,
National Cancer Centre Singapore. He specialises in breast oncology, neurooncology
and the use of stereotactic radiosurgery for both benign and malignant
indications.
He is active in research in breast cancers and has published in several peer-reviewed
journals. In his educator role, he has mentored students from medical students to
specialist trainees under his care, and regularly lectures at Nanyang Polytechnic for
Allied Health students.
