All surviving patients have been alive for more than two years after they received the treatment.PHOTO: ST FILE
Some lymphoma patients suffering from an aggressive form of blood cancer have shown positive response to a certain type of immunotherapy, according to researchers from the National Cancer Centre Singapore (NCCS).
Immunotherapy is a type of cancer treatment that activates the immune system to fight the disease.
The researchers from NCCS found that patients with Natural-Killer T-Cell Lymphoma (NKTCL), a rare but aggressive type of blood cancer, responded well to anti PD-1 immunotherapy if they had a mutation in their PD-L1 gene.
Their findings were published in medical journal Leukemia on Aug 5.
The PD-1 and PD-L1 genes are known as checkpoint proteins on the cells' surface and together form the immune checkpoint.
These proteins help regulate the immune system during infections, preventing over-activation of the system, which could cause host tissue damage.
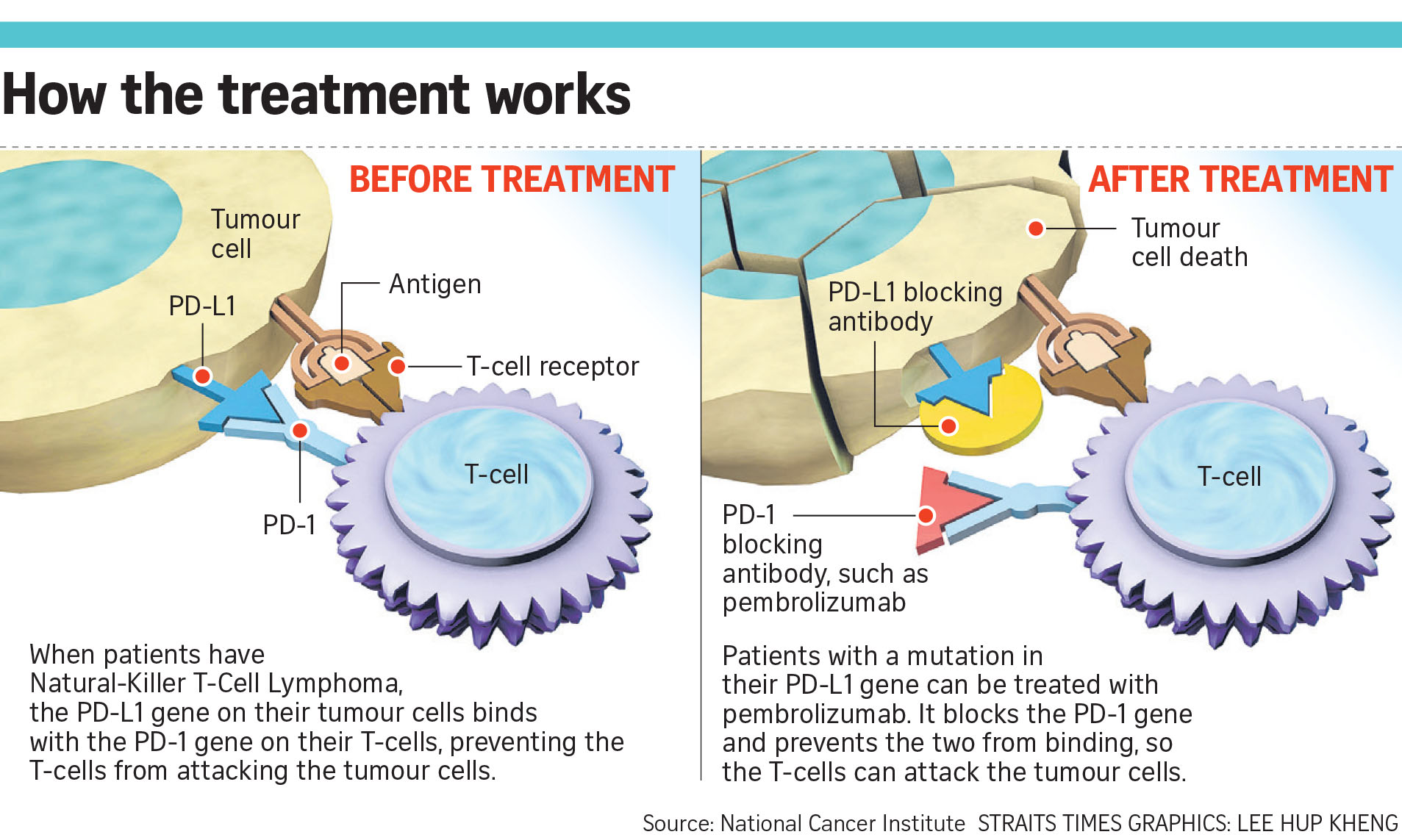
However, in the case of NKTCL patients, the PD-L1 gene on the tumour cells binds with the PD-1 gene on the T-cells, preventing the T-cells from attacking the tumour cells.
The anti PD-1 therapy, which is an immune checkpoint inhibitor, works by blocking the two proteins to stop them from binding, thus activating the T-cells to launch an attack on the tumour.
Pembrolizumab is an anti PD-1 monoclonal antibody which blocks the PD-1 gene, disrupts the immune checkpoint and activates the T-cells.
This antibody, which has recently been used for lung cancer treatment, was utilised in the NCCS study. Subsequently, seven out of 19 NKTCL patients saw complete recovery.
In the study, local researchers collaborated with researchers from China, Hong Kong SAR and South Korea to study relapsed patients who were treated with pembrolizumab.
Four of these recovered patients had a mutation in their PD-L1 gene, which the researchers believe is the reason for their treatment's efficacy. All surviving patients have been alive for more than two years after they received the treatment.
Dr Ong Choon Kiat, principal investigator of the division of cellular and molecular research at NCCS' Lymphoma Genomic Translational Laboratory, said: "The study of how NKTCL patients respond to immunotherapy has been limited to date. We are pleased that our study has identified robust biomarkers that reliably improve treatment selection for patients who will have a high likelihood of responding positively."
The team filed a patent for the technology in 2017 and a diagnostic test was developed by local biotech company Lucence Diagnostics to determine which patients will be able to benefit from the treatment.
In the test, DNA from the tumour sample is extracted to detect the presence of mutation in the PD-L1 gene.
All patients who have relapsed or are no longer responding to chemotherapy or radiotherapy will be offered the diagnostic test to see if they will benefit from pembrolizumab.
The drug is administered through an intravenous injection every three weeks and the treatment continues as long as the patient is benefiting from it.
Current studies are looking into the optimal duration of therapy, which has not yet been determined with certainty.
Professor Lim Soon Thye, deputy medical director (clinical) of NCCS and a principal investigator of the study, said: "Guiding the choice of therapy is critical for cancer patients, where treatment must be timely and drugs can be costly.
"It is not easy to bridge the gap from bench to bedside, so it is particularly gratifying to be able to translate our findings into clinical applications that will directly benefit patients and healthcare systems."
ABOUT LYMPHOMA
Lymphoma is a cancer that starts in a type of white blood cells known as lymphocytes.
In a patient suffering from the disease, the lymphocytes multiply uncontrollably and fail to die like normal cells.
There are two types of lymphocytes: T-cells and B-cells.
atients with lymphoma typically experience swelling in the lymph nodes in their neck, underarms or groin, a result of painless lumps or tumours forming.
Other symptoms include persistent fevers, night sweats and unexplained weight loss.
In order to diagnose lymphoma, doctors conduct blood tests to determine blood cell, kidney and liver performance, as well as a bone marrow biopsy to examine abnormal B-cells or T-cells.
T-cell lymphoma, a type of non-Hodgkin's lymphoma, affects the T-cells in the immune system.
It can either be slow-growing or aggressive - in the latter case, the cancer grows and spreads quickly, causing severe symptoms.
Natural-Killer T-Cell Lymphoma, in particular, is known to be a rare and aggressive cancer with no targeted therapy options.
Due to the cancer's aggressive nature, the three-year overall survival rate among patients is under 30 per cent.
The cancer is more prevalent in Asia and is seen more frequently in China and Japan.
It is rarer in Singapore, with fewer than 20 cases each year.
Patients often undergo a standard treatment, combining chemotherapy and radiotherapy, though they tend to relapse and the treatment is not able to guarantee survival beyond six months.
Hence the possibility of immunotherapy - such as using monoclonal antibodies to boost the immune system - continues to be explored.
