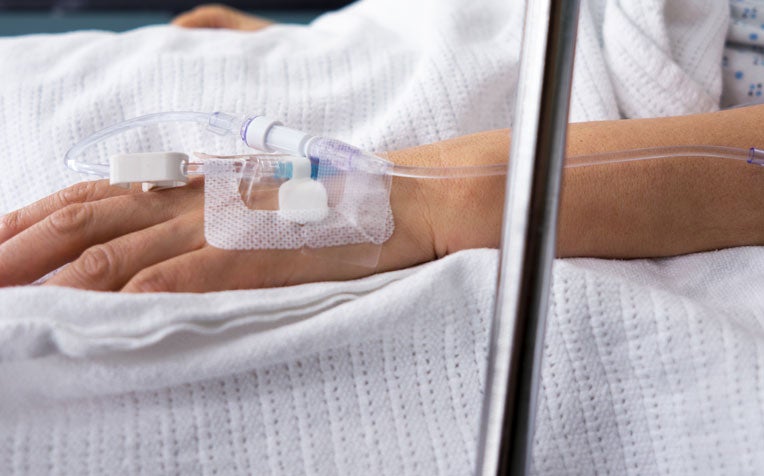
The Intensive Care Unit (ICU) provides the support and resources vital for a patient's survival.
It’s 9pm on a Monday. The phone rings but the number displayed is unfamiliar. “I’m Staff Nurse Yang* from Singapore General Hospital (SGH). May I speak to Mrs Ho* please? It’s about her mother.” Mother, in her late 70s, is generally healthy. “Yes, I am Mrs Ho.” Staff Nurse Yang tells you that your mother has been admitted to the intensive care unit (ICU). Her condition is worsening and she may not survive the night. You have to go to SGH immediately.
Having a loved one diagnosed with a life-threatening illness can haunt the patient’s family and close friends for years. Research has found that many relatives suffer long-lasting psychological effects similar to post-traumatic stress disorder.
At the ICU, you are told to wait while important procedures are done. After what seems like an eternity, you are allowed to see your mother. Surely an exception could have been made under the circumstances?
On a typical day at the ICU, up to 100 procedures are performed on a critically ill patient. These include checking various parameters like blood pressure, breathing rate and oxygen level, suctioning secretions from lungs, turning the patient to prevent bed sores, emptying urine bags, and inserting the various tubes which help keep the patient alive. There are also trips to the scanning rooms or operating theatre. Only when there is a lull in these activities can visitors see the patient.
The sign on the door says “Contact precautions”. The nurse asks you to put on a special gown and gloves before entering Mother’s room. You are shocked by her appearance. The monitor at her bedside displays rainbow-coloured waves and numbers. One reading is for her heart rate and blood pressure. But what are the others? Every now and then, an alarm rings and a number flashes. The intensivist (intensive care specialist) explains that Mother is on a life support machine to help her breathe because she has a serious chest infection. It is very difficult to tell how she will do at this stage.
The ICU was introduced in the 1950s to provide life support, primarily of the breathing system, during the polio epidemic of that period. Today, it caters to the care of almost every major organ system including the heart, kidneys and lungs. If a disease worsens and overwhelms the body, the patient’s vital organs will start to fail. Organ support keeps him alive by buying precious time for the body to recover. During this time, the patient’s condition can be volatile, and swings in his parameters will trigger alarms.
“Mother,” you call out. You detect a faint movement in her eyes and hands but is she aware of your presence? You recall your happy times together, and wonder why you haven’t spent more time with her. You want to reach out and hold her hand but are reminded of the ‘Contact precautions’ warning. Why is she still unconscious? Can we wake her up? I have so much to say to her.
The breathing tube is one of the most uncomfortable devices for a patient in the ICU. Our natural instinct is to pull it out. Sedation provides some relief from the pain and discomfort associated with this and the various other life support measures necessary to help recovery.
During a critical illness, the immune system which protects us from bacteria and viruses may be weakened, allowing infections to occur and create havoc. A worrying trend is that many of these infections don’t respond to antibiotics. The use of special gowns, masks and gloves helps minimise the spread of germs to vulnerable patients.
Days become weeks and visiting the hospital has become routine. One day, the doctor says Mother is on the mend. But the next day, her condition worsens. Last week, it was a new urinary tract infection. This week, it is bleeding from the stomach. It’s all very confusing and worrying.
When severe illness strikes, it leaves the body vulnerable to other problems and complications. What is harmless to healthy people can seriously threaten a critically ill patient and compromise his ability to recover.
After a particularly stressful week, Mother begins to improve. She regains consciousness, but cannot speak because of the breathing tube. A writing board is used for communication. Soon, she is able to breathe on her own – albeit through a tube inserted via an opening in her neck. Finally, she is transferred to the high-dependency ward!
For every 10 patients who enter the ICU, seven to nine survive. Despite advances in medical science, many ICU patients do not survive.
Mother returns home but her body carries the marks of her illness. She has a scar on her neck – a reminder of the breathing tube that was used to help her breathe. Minor exertions like taking a shower leave her short of breath. Her condition will improve with rehabilitation but the pace of recovery will be slow. So you remind yourself to be patient.
Many patients who survive the ICU struggle with long-term disabilities because of scarring in the lungs, stroke, muscle weakness or mental impairment. Despite the many formidable challenges that ICU survivors face, many of them show remarkable resilience and learn to adapt to what others may consider insurmountable difficulties. These are the patients who serve as an inspiration for the people who work in intensive care.
Ref. Q15
Contributed by

















