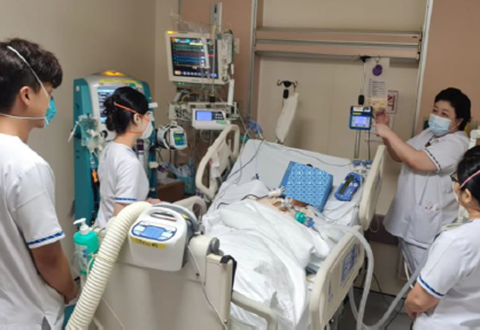
Nutrition plays an important part in everyone’s lives, even more so for critically ill patients.
At the Cardiothoracic Intensive Care Unit (CTICU), post-surgical patients begin to receive nutrition within 24 hours after admission – either orally or via continuous enteral feeding (delivering of feeds via nasogastric tube into the stomach) for intubated patients.
“Studies have shown that adequate nutritional intake can reduce infectious complications, length of stay and mortality especially for post-surgical patients, improving overall outcomes,” shared Senior Nurse Manager Yeoh Lee Shien from CTICU.
Identifying the issues
Lack of standardised practices
For patients on enteral feeding, nurses are required to check the Gastric Residual Volume (GRV), the amount aspirated from the stomach following the administration of enteral feeds. Knowing the GRV aids doctors in assessing patient’s tolerance towards feeding and also helps protect patient against aspiration pneumonia – a condition when food or liquids is breathed into the lungs or airways leading to the lung, instead of going through the esophagus and stomach.
Nurse Clinician (NC) Tan Sin Yain who led the Revivors team said, “There was no standardised protocol for enteral nutrition and GRV management. Nurses check the GRV either four-hourly or at random times while doctors tend to use their own clinical judgement for assessment. She added that patients with raised GRVs are referred to SGH’s Nutrition Support Services (NSS) for further assessment and while awaiting outcome, their enteral feeds may be stopped for up to 24 hours.
“When feeds are stopped, patients may experience certain risks - malnutrition which will delay recovery, hypoglycemia leading to unresponsiveness, or arrhythmia due to electrolytes imbalance,” shared Asst Prof Tan Teing Ee, member and Head, Department of Cardiothoracic Surgery.
Unnecessary referrals
In 2019, the team received feedback that half of the referrals to NSS were unnecessary. “We looked into the data and discovered that referrals had doubled from 2018 to 2019 with time and resources wasted on unnecessary referrals,” shared NC Tan.
Improving quality of care
Formalising guidelines and practices
The team came up with standardised guidelines on continuous enteral feeding and GRV checks. The criteria for referrals to NSS was also developed. These were formalised into a policy and made readily available on the intranet. A handy hardcopy version was attached to the Computer on Wheels (COWs) in the ward for easy reference.


Clear guidelines and workflows guide the care team in managing the patient’s feeds better.


Doctors and nurses were briefed and trained via roadshows, roll-calls and regular huddles.
Preventing complications
Another area of concern raised by the medical team was the possible complications that could occur when using certain drugs to improve patient’s digestion of feeds.
“When we see that patients have issues digesting their feeds and hence, not absorbing their nutrition well, certain drugs may be used to help them digest and absorb their feeds better. At times, complications such as abnormal heart rhythm could potentially occur. To manage this, we worked with Pharmacists to include alternative medicine as a preventive measure,” shared member, Advanced Practice Nurse Gillian Wee.


(L-R) Alternative medicine for patients with potential arrhythmia problems; In addition to Pharmacist, a senior doctor is assigned to the care team as resource persons when the team has doubts relating to medicines or care management.
Reaping results
After the measures were fully implemented in the second quarter of 2019, the team successfully brought the number of unnecessary NSS referrals to zero. This result has sustained till-date.
“The elimination of unneeded referrals has translated to substantial cost savings for patients and NHCS. More importantly, the knowledge and guidelines put in place by the team strongly empowered us to better care for patients, ensuring they are ‘well fed’, and hence recover better and faster!” shared member, Senior Staff Nurse (SSN) Xiao Bing.
The Revivors team clinched the Gold Award at the Team Excellence Symposium organised by Singapore Productivity Association.












