Singapore General Hospital's new isolation facility is a much needed boost in capacity to support the nation's fight against COVID-19 and other infectious diseases.
The squat, single-storey building with its canvas roof may seem at odds with its more richly endowed neighbour, the historic and grand Bowyer Block. But the building, looking more like army barracks or a marquee, serves an important purpose — and is creating its own history.
Sitting on a former car park, the 3,200-square-metre building is Singapore General Hospital’s (SGH) newest ward. It is not just any general purpose ward, but one that houses patients who need to be isolated during infectious disease outbreaks. Indeed, when the idea for Ward@Bowyer, or Ward 88, took shape in April 2020, it was at the height of the COVID-19 pandemic in Singapore.

<<Associate Professor Ruban Poopalalingam, Chairman, Medical Board, SGH.>>
“It was part of the national plan to increase capacity to deal with the COVID-19 outbreak,” said Associate Professor Ruban Poopalalingam, Chairman, Medical Board, SGH.
At the time, SGH and other hospitals were stretched beyond their capacity and no one could predict how long the COVID-19 pandemic would last. “So there was a real need at that point to set up this ward,” Prof Ruban said.
The ward, though not meant to be permanent amid various expansions on SGH Campus, has increased the number of isolation rooms and can be used beyond the COVID-19 pandemic, such as during other infectious disease outbreaks like seasonal flu, measles, and tuberculosis. When these outbreaks stabilise, Ward@Bowyer can also be used for non-infectious cases. The ward, said Prof Ruban, “would be a good place to house patients until we know exactly what we are dealing with”.

<<Ward@Bowyer, built on an open-air car park, is a significant addition to the hospital’s capacity to handle patients with infectious diseases.>>
In late August when the number of infections fell, COVID-19 patients were housed back at Ward 68, SGH’s regular isolation ward. Ward@Bowyer was then used for patients who needed to be isolated to prevent airborne diseases, such as varicella zoster virus (chicken pox) and pulmonary tuberculosis, which are spread through respiratory droplets.
The ward was not modelled after the hospital’s existing isolation ward, which was based on the lessons learnt during earlier disease outbreaks, such as severe acute respiratory syndrome (SARS). Instead, to meet the urgent need for additional isolation rooms at the time, pre-fabricated isolation cabins were used.
Each of the 50 units was pre-fitted with toilets, showers, and other appliances necessary for patients who are infectious and need to be isolated. Put together with minimal construction, which started in mid-May, the ward admitted its first patients on 15 July 2020. It also added to Ward 68’s then isolation facility comprising 35 single rooms and 16 beds in shared rooms.
The number of suspected and confirmed COVID-19 cases at SGH ranged from 200 to 300 at any one time during the peak of the COVID-19 outbreak in April and May. Before Ward@Bowyer, wards had to be converted for isolation patients during that period.
Prof Ruban said that SGH had to constantly decide how much of the hospital should be used for COVID-19. “We had to balance between patients who needed care and were not related to COVID-19, and COVID-19 suspected and confirmed cases. Having these extra 50 isolation rooms was really useful in helping us strike a better balance,” he said.
The ward is run by a team of 40 nurses trained in intensive care and infection control, led by Ms Thurgathavi P Vellasamy, Nurse Clinician, SGH. The nurses came from different wards, with Ms Thurgathavi originally from the Colorectal Surgical ward.
“When we first came together, we underwent orientation that included understanding the use of the facilities and infection control practices, as well as simulations to ensure that we are able to provide the care that patients in this ward need,” Ms Thurgathavi said.
An important feature of the ward is its layout. It had to consider workflow and processes that allow care to be delivered efficiently and safely. For instance, the two-way lockers in the staff rooms are designed to allow the ward staff to shower after their shifts to avoid carrying germs into the community.
During the COVID-19 outbreak, the ward was divided into three zones. The creation of the zones — for patients with acute respiratory infections, suspected COVID-19, and confirmed COVID-19 infections — was an added precaution to lower the risk of cross-contamination.
A glimpse into Ward@Bowyer


Each isolation unit measures 2.3m by 5.6m with a height of 2.5m. The negative-pressure room ensures that viral particles do not escape when the door opens. Oxygen is pumped into the room while the air inside is expunged through a high-efficiency particulate air (HEPA) filter at the foot of the bed. Toilet waste is treated before being discharged to regular sewers.

Patients who need to have x-rays taken are brought to an on-site booth called SG SAFE.R, which is designed by SGH’s Department of Diagnostic Radiology. Made from high-performance polycarbonate plastic panels, the booth is operated by only one radiographer. The patient stands in the booth with his or her body pressed against the x-ray plate, while the radiographer operates the x-ray machine outside the booth, protected by a lead shield that absorbs radiation. As the radiographer and patient do not come into contact, the former wears just an N95 mask. After each session, the booth is disinfected by a healthcare assistant donning personal protective equipment.

Every patient is given an admission pack containing a digital thermometer, surgical masks, and toiletries, as well as drinks and snacks.

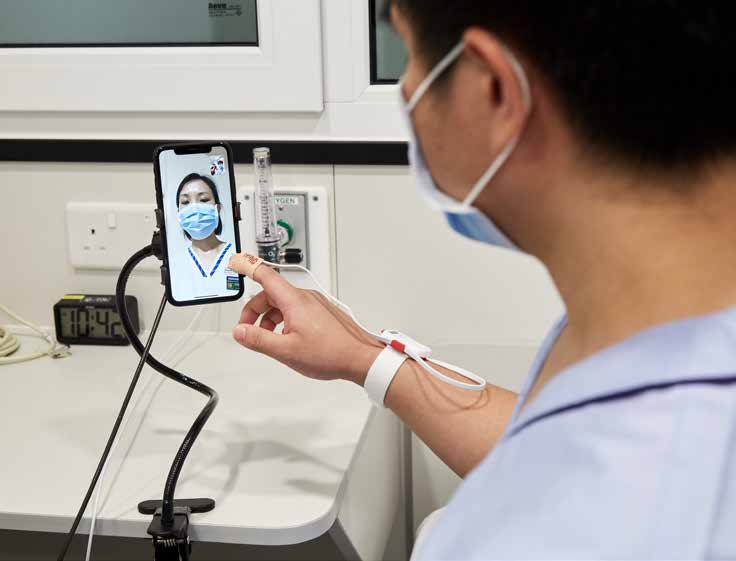
A biosensor worn on the wrist monitors round the clock his vitals, such as heart and respiration rate, and oxygen saturation levels, with the information transmitted to the medical team for remote monitoring. The data are also available via an app on a smartphone that is given to each patient. Other apps let the patient communicate with the team. Games and multi-language reading materials are also pre-loaded into the phone. For patients who cannot speak local languages, a picture board in the room helps with some basic words to help them communicate with the medical team.

Developed with recommendations from SARS experts, the Treatment Room is equipped to provide emergency care. It takes about one minute for first responders to transport a patient from an isolation unit to the room. In a Code Blue situation, the team stationed outside the ward will arrive in five to seven minutes. Patients who require further resuscitative or intensive care will be transferred to SGH wards.













 Get it on Google Play
Get it on Google Play