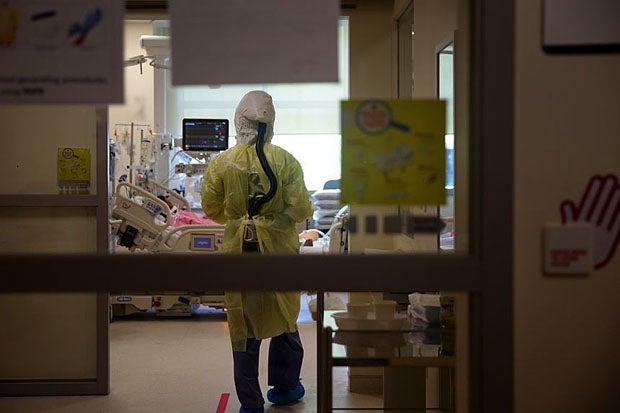
Hospitals had started planning for more Covid-19 beds after large clusters emerged, fuelled by the Delta variant.PHOTO: ST FILE
SINGAPORE - Serious Covid-19 cases are unlikely to overwhelm intensive care unit (ICU) capacity in Singapore, as hospitals here work to strike a balance between the needs of severe coronavirus cases and other critical care patients.
In an interview with The Straits Times, Professor Dale Fisher, a senior consultant in infectious diseases at the National University Hospital, said hospitals have measures to deal with the potential surge in high-risk or serious cases.
They involve managing the beds for these patients, the supply of personal protective equipment, ventilators and drugs, as well as the staff needed to care for them.
He also pointed to the vaccination rate in Singapore - as at Wednesday, 73 per cent of the population are fully vaccinated. Fully vaccinated people are less likely to fall seriously ill.
"It's almost impossible for our capacities to become exhausted because it's a very controlled situation," said Prof Fisher.
"We watch daily how many people have severe disease. We also see most recover and we know also that each day, over 50,000 people are having their second jab, thereby approaching full immunity status."
But one area of concern remains - the elderly.
Ministry of Health (MOH) figures show that as at Aug 5, about 80,000 of those aged 70 and above had yet to be vaccinated.
Prof Fisher said hospitals can make some predictions by seeing the number of elderly unvaccinated patients with mild disease. He added that it takes about a week for severe disease to show.
"If any of these indicators reach concerning levels, then we could see strengthened community measures," he said.
As at Thursday (Aug 12), there were 470 Covid-19 patients in hospital, including 36 who required oxygen supplementation and nine in the ICU.
Hospitals had started planning for more Covid-19 beds after large clusters emerged, fuelled by the highly contagious Delta variant.
The Jurong Fishery Port cluster, which saw the virus spread rapidly to markets and hawker centres last month, was especially concerning. With 200,000 seniors yet to take the jab at that point, the worry was that many unvaccinated elderly people would end up in the ICU.
Health Minister Ong Ye Kung reassured the public, saying that up to 1,000 ICU beds can be made available for critically ill Covid-19 patients if needed.
At Alexandra Hospital (AH), two wards were turned into Covid-19 wards between late April and last month.
Its chief operating officer Jeffrey Chun said the hospital will also renovate a general ward early next year to equip it with negative pressure rooms that can be quickly turned into ICU rooms for Covid-19 patients. These rooms are built to handle additional equipment and have more power points than normal rooms.
Dr Liew Mei Fong, director of the hospital's ICU, said: "There will be provisions for more equipment such as mechanical ventilators, invasive monitors, continuous cardiac monitoring and dialysis machines, to name a few."
She said ICU doctors have completed intensive care medicine training, on top of their own speciality training. Nurses in the ICU also undergo specialised training.
"The typical staff ratio would be one nurse to one patient for an ICU patient, and one nurse to two patients for a high dependency patient," added Dr Liew.
At Singapore General Hospital (SGH), some non-urgent elective procedures are being rescheduled to create capacity for clinical care.
Associate Professor Ruban Poopalalingam, chairman of SGH's medical board, said: "This allows us greater flexibility to deploy manpower to support areas with pressing needs."
The hospital, he added, can quickly turn rooms into negative pressure ones by installing a portable anteroom, should isolation rooms or wards be fully occupied. This is a chamber-like system to prevent contaminated air from escaping the room.
SGH has another 50 isolation units at Ward @ Bowyer, the facility it built last year at an open-air carpark on hospital grounds.
Prof Poopalalingam said more general wards can be converted into Covid-19 wards if need be.
AH's Mr Chun said it is a "tight balancing act" of ensuring enough beds for Covid-19 patients while making sure that other patients have access to the care they need. "This is the reason why we keep a constant and close watch on Covid-19 case numbers and flex our wards accordingly, working closely with MOH and the rest of the hospitals."
Contributed by













