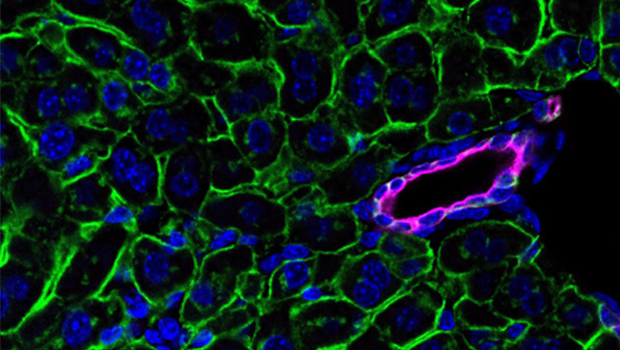
Omega-3 lysolipids are important for protecting the liver from dietary fat, according to Duke-NUS researchers and collaborators from SGH. Detection of the lysolipid transporter Mfsd2a in hepatocytes, stained green, in proximity to a bile duct, stained magenta(Credit: Chin Cheen Fei).
Long-running research by Duke-NUS Medical School into the omega-3 transporter protein Mfsd2a has shown that it plays a key role in a specific mechanism that prevents the liver from storing too much fat from food. Published in the Journal of Clinical Investigation, this latest study by Duke-NUS and collaborators from Singapore General Hospital (SGH) signals the possibility that a dietary supplement could be developed to help prevent non-alcoholic fatty liver disease (NAFLD).
Eating too much fatty food increases the risk of many health problems, including cardiovascular disease, obesity, diabetes and NAFLD. The excess fat that accumulates in the liver during the onset of NAFLD leads to inflammation and progressive deterioration and scarring, called cirrhosis of the liver. The rate of NAFLD is remarkably high in Singapore, affecting around 40 per cent of adults compared to 27 per cent globally.
One type of fat called phospholipids are essential for making cell membranes and actually protect the liver against the harmful effects of dietary fat.
"For over a decade, the researchers at Duke-NUS have been studying Mfsd2a, which transports the phospholipid lysophosphatidyl choline (LPC) into cells," said Dr Chin Cheen Fei, first author of the study and Research Fellow with Duke-NUS' Cardiovascular & Metabolic Disorders (CVMD) Programme. "In this latest work, we set out to determine if LPC transport into the liver by Mfsd2a is an important source for liver phospholipids and a means of protecting the liver against NAFLD."
The team embarked on studies using preclinical and isolated samples of human liver. They focused on the effect of a variety of measures that altered the activity of Mfsd2a and its uptake of specific lipids.
"Our findings show that LPC lipids, particularly those containing polyunsaturated fatty acids such as omega-3 fatty acid DHA, could become a means of long-term prevention for NAFLD," said Dr George Goh, Senior Consultant at SGH and one of the collaborators of the study. "Our study is the first to suggest the potential of dietary LPC supplementation in protecting the liver against damage caused by a high-fat diet."
The researchers noted that the liver has a significant demand for phospholipids in general, which increases when challenged with fatty foods. NAFLD takes years to develop and can progress to non-alcoholic steatohepatitis and cirrhosis, so supplements taken over that period could offer protection.
"Our study emphasises the importance of taking a proactive approach to keeping the liver healthy," said Professor David Silver, the senior author of the study and Deputy Director of the CVMD Programme. "Overnutrition with fatty foods can cause cardiovascular disease, obesity, diabetes and NAFLD. The prevalence of NAFLD is of major importance to the general population, which is becoming increasingly aware of this problem."
As the discovery marks a significant development in the search for a way to protect liver function from a disease that is affecting a growing number of people across the world, the Duke-NUS research team now plans to undertake rigorous clinical studies with their collaborators at SGH to test whether LPC supplementation really can improve the outcomes in patients with NAFLD.
"If the trials prove successful, this work could help the vast numbers of people worldwide whose health is seriously affected by the condition," said Prof Silver.
Next, the team plans to probe in more detail the molecular mechanisms that allow LPCs to promote liver health in general.
Professor David Silver, Deputy Director of Duke-NUS' Cardiovascular & Metabolic Disorders (CVMD) Programme, and Dr Chin Cheen Fei
Reference: Chin, C.F. et al. (2023) Blood-derived lysophospholipid sustains hepatic phospholipids and fat storage necessary for hepatoprotection in overnutrition, The Journal of Clinical Investigation. Available at: https://www.jci.org/articles/view/171267
Get updates on Tomorrow's Medicine in your mailbox!












