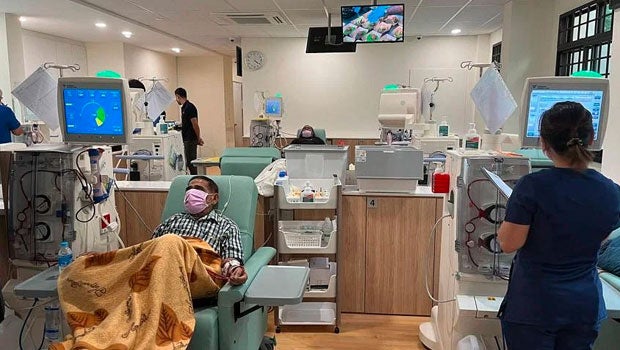
Kidney failure is a global epidemic with about 850 million people suffering from it. PHOTO: ST FILE
SINGAPORE – Patients with kidney failure may be able to reverse the damage, if a new treatment is proven to be as good in humans as it is in mice. Safety trials in humans will start in 2023, and if all goes as well, clinical trials in patients will begin in the next two to three years.
“This discovery could be a real game-changer in the treatment of chronic kidney disease – which is a major public health concern in Singapore and globally – bringing us one step closer to delivering the benefits promised by regenerative medicine,” said Professor Thomas Coffman, dean of Duke-NUS Medical School, and a member of the research team.
The team from Duke-NUS Medical School, National Heart Centre Singapore (NHCS), and researchers from Germany, were able to inhibit a protein which plays a major part in organ damage, resulting in the injured kidneys regenerating and renal function restored.
The team said this is a first in the world, where treatment has enabled damaged kidneys to regenerate. They had been working on this project for more than a decade, not just in kidneys but also other organs like the lungs and liver.
Kidney failure is a global epidemic with about 850 million people suffering from it, said Assistant Professor Anissa Widjaja, a molecular biologist with Duke-NUS’ Cardiovascular and Metabolic Disorders Programme. Kidneys can be damaged through acute infections or chronic diseases such as diabetes. She said Singapore ranks first in the world for diabetes-induced kidney failure and fourth in terms of kidney failure prevalence.
The researchers said kidneys have the innate ability to regenerate.
They gave mice with inflamed and scarred kidneys a neutralising antibody against the interleukin-11 (IL-11) protein, which is known for causing damage and scarring in organs such as the kidneys, liver, lungs and heart.
The treatment targeted the cells on the lining of the tiny tubes inside the kidney that return nutrients into the body, leaving urine behind. When treated with the neutralising antibodies against IL-11, the tubule cells were able to proliferate and regenerate the kidney, reversing the damage.
There was improvement in all the mice, no matter how badly damaged the kidney was.
The results of the pre-clinical study were published online in the Nature Communications journal in December 2022.
“The therapy could be used to treat people at risk of acute kidney disease to prevent it, to treat people who have acute kidney disease to reduce kidney damage, and to treat patients with established chronic kidney disease to reverse it. This is because activating regeneration in the kidney is useful across all types of kidney disease,” said Professor Stuart Cook, a cardiologist with the Duke-NUS’ Cardiovascular and Metabolic Disorders Programme as well as a clinical scientist at the NHCS.
Prof Cook, who was the principal investigator of the study, said: “We showed that anti-IL-11 therapy can treat kidney failure, reverse established chronic kidney disease, and restore kidney function by promoting regeneration in mice, while being safe for long-term use.”
Testing the antibody in healthy humans will begin early in 2023. If that goes well, clinical trials in patients should begin in 2024. These will be done by pharmaceutical giant Boehringer Ingelheim, whose researchers were involved in the study, as it has purchased the licence to do so. The trials in humans are likely to start with patients with fibrotic lungs, with trials among kidney patients coming next.
The experiment in mice involved a number of cohorts over several years, to ensure “robustness” in the results. To test its effectiveness against chronic kidney disease, the kidneys in mice were “badly damaged” to lose about a third of their function. After about three weeks to stabilise the damage, the mice were injected with the antibody.
Over a period of three months, the treatment resulted in more than 50 per cent reversal of kidney dysfunction and fibrosis, and the kidneys were visibly “growing back”, said Prof Cook.
The experiments on mice stopped after three months of treatment. If it had been prolonged, he said, there may have been even more improvements.
Prof Cook said the chance of anti-IL-11 working in humans is high, since the study was also carried out on human cells, with the same outcome.
Asked if the regeneration would work as well in older mice, and hence older humans, Prof Cook said yes, based on further experiments, the results of which have yet to be published. “The antibody works in old mice with kidney disease as well as in mice that have kidney disease and diabetes,” he said.
However, the treatment, when it becomes commercial, is likely to be “reasonably expensive”, said Prof Cook, but he added: “The cost of giving a drug that prevents someone going onto kidney dialysis is very small compared with the cost of dialysis itself.”












