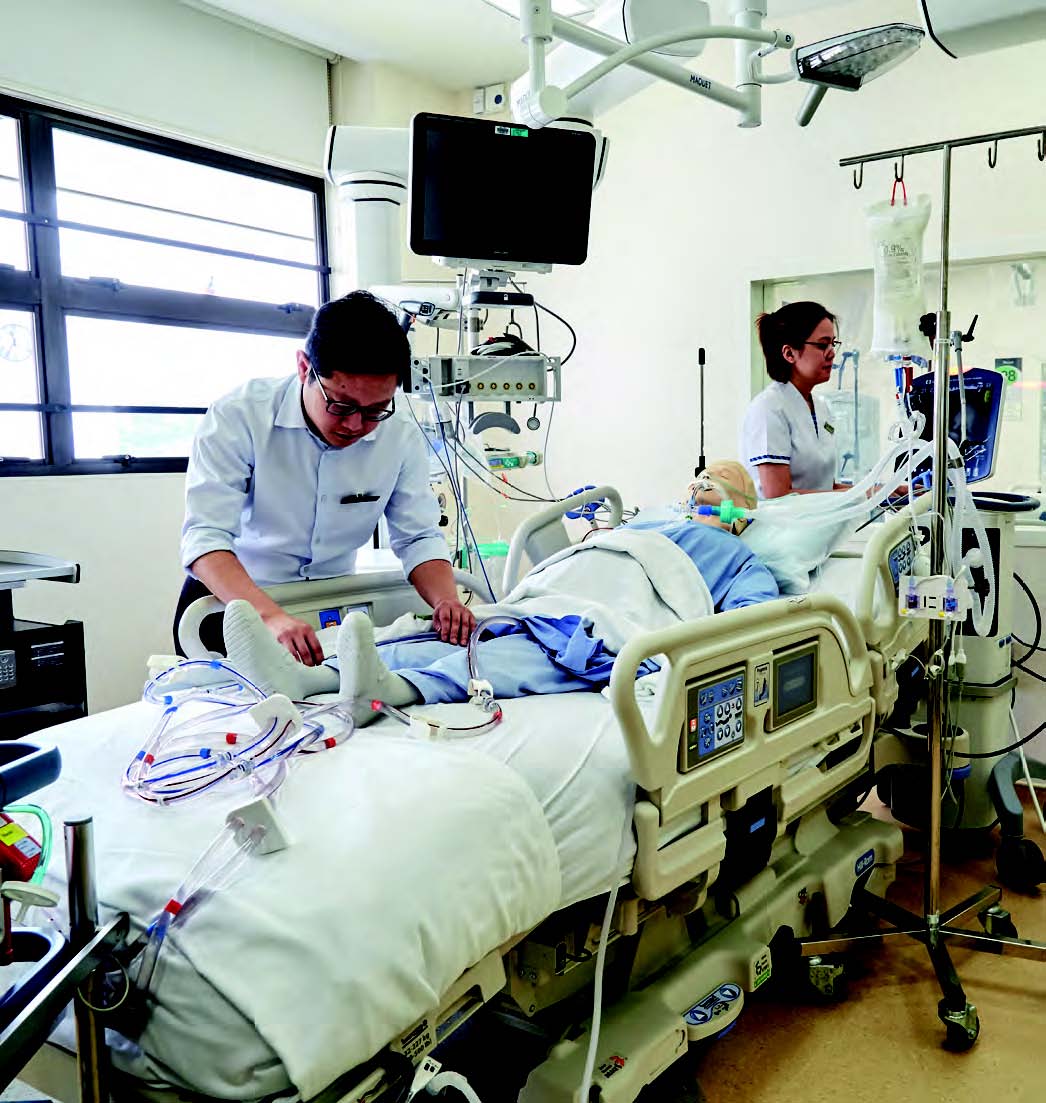
Dr Sewa Duu Wen sets up the extracorporeal membrance oxygenation (ECMO) machine on a mannequin. ECMO delivers oxygen into the bloodstream without injuring the lungs.
When ICU mechanical ventilators are inadequate, respiratory ECMO can temporarily replace the functions of the lungs to oxygenate blood and remove carbon dioxide.
Thinking it was just a regular flu bug, Mr Heng Wee Heng, 19, popped a few paracetamol tablets and waited for his symptoms — high fever and cough — to pass. Instead, his illness worsened and, within days, he was admitted to a hospital’s intensive care unit (ICU) with severe pneumonia.
At the ICU, Mr Heng was hooked up to a mechanical ventilator machine to help him breathe. But doctors were concerned the intense ventilator support might hurt his lungs, and he was recommended extracorporeal membrane oxygenation (ECMO) therapy, where oxygen is delivered directly into the bloodstream, bypassing the lungs.
Mr Heng was then sent to Singapore General Hospital (SGH), one of two public hospitals offering the treatment.
“ECMO is life support therapy for patients with acute reversible lung disease. If their conditions are still deteriorating even when they are on conventional mechanical ventilator support, they could be at risk of dying of severe lung failure,” said Dr Phua Ghee Chee, Senior Consultant and Head, Department of Respiratory and Critical Care Medicine, SGH.
“ECMO is used as rescue therapy. ECMO is not a cure. It supports patients, and acts as a bridge for the lungs to recover,” he added.
Patients like Mr Heng with severe pneumonia or respiratory failure need intensive ventilator support. Pushing oxygenated air at very high pressures into the lungs over an extended period can injure the organ, said Dr Sewa Duu Wen, Senior Consultant, Department of Respiratory and Critical Care Medicine, SGH.
“With ECMO, we are able to reduce the intensity of the mechanical ventilator and give patients a higher chance of surviving the episode,” said Dr Sewa, who is also Director of the Medical Intensive Care Unit (MICU) at SGH.
Better survival chances
Nevertheless, ECMO isn’t without its risks; and while it can save lives, it isn’t for everyone.
Patients have to be carefully selected to make sure that they are able to tolerate ECMO, which has been associated with complications, such as bleeding, blood clots, stroke, infection, kidney failure, and even death.
The ECMO service at the MICU was introduced in 2009 during the H1N1 pandemic. Since then, the team has been progressively increasing the capability and expertise of the ECMO service.
Two years ago, the service was reorganised and a large multidisciplinary ECMO team is now available round the clock. The team includes ECMO-trained physicians and nurses, cardiothoracic surgeons, perfusionists, respiratory therapists, intensive care pharmacists, physiotherapists, and medical social workers.
According to Dr Phua, before 2018, an average of eight patients underwent ECMO a year, and the survival rate was about 60 per cent. Survival rates are now more than 80 per cent, he said.
About 50 per cent of patients treated with ECMO at SGH come from other institutions. The youngest person treated at SGH was 16 years old. Patients stay on ECMO for about six days (although they are at the MICU for about two weeks), before being moved to the wards to stay another 25 days or so.













 Get it on Google Play
Get it on Google Play