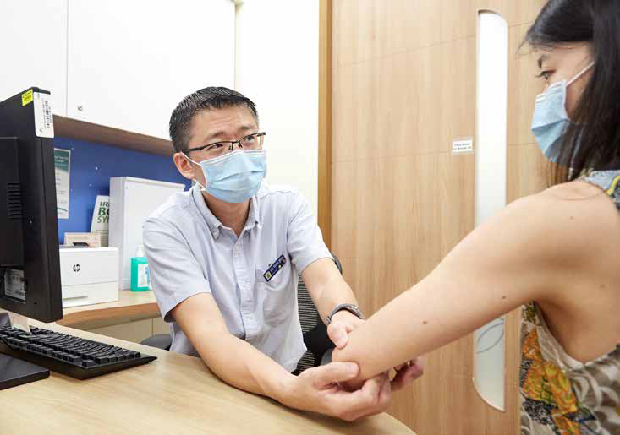
It was a good thing that pride and fear did not stand in Singapore General Hospital (SGH) pharmacist Mr Lim Teong Guan’s way for long. Otherwise, he would not have been among the first pharmacists in Singapore to be able to prescribe medicine for patients. Pharmacists can — and do — suggest changes in patients’ prescriptions, but attending doctors have to review and approve their recommendations. Only pharmacists who have undergone and passed the Ministry of Health’s (MOH) collaborative prescribing programme introduced in 2018 can prescribe medications to patients independently.
The MOH programme involved a day each week of teaching, which included case-based discussions, lectures, clinical simulations, and hands-on practice. Participants also had to accumulate 80 hours of clinical practice before being allowed to take the final examination. While SGH allowed the pharmacists time off to attend the weekly lessons, the 14-week programme was still very intense, said Mr Lim, Senior Principal Clinical Pharmacist.
“Then there was the matter of pride. After 18 years of practice, it would be very embarrassing if I failed to pass. No face!” Mr Lim said.
He initially waited “to see who would jump into the sea first and swim”. After further thought, he decided that “as the pharmacist in charge of outpatient clinical service, I felt I had to take this leap and lead by example. I cannot ask my team to swim without me swimming first”.
Collaborative care
He goes on ward rounds as part of a multidisciplinary team, and runs the Rheumatology Monitoring (RM) and Inflammatory Bowel Disease clinics. At these clinics, he functions pretty much like a doctor: he takes patients’ medical history, performs physical examination, discusses treatment plans, orders investigations, and prescribes medications.
During the COVID-19 crisis, the RM clinic adopted teleconsultation to minimise the length of each patient’s hospital visit. Patients just need to have their blood tests done at SGH or SingHealth Polyclinics, then the collaborative pharmacist reviewed the results with the patients over the phone, followed by prescription and arrangement of medication delivery.
Running these clinics means doctors can focus their attention on patients with more complex conditions. Patients, too, benefit as clinics are less crowded so they are seen faster.
“For our healthcare system as a whole, collaborative prescribing practice is an efficient way of utilising scarce healthcare resources. It enables Singapore to set the standard of practice for regional countries to follow,” said Mr Lim.
Mr Lim and other pharmacists who underwent the course have become more confident in identifying symptoms and making diagnoses. Although he is busier than before — he also has administrative duties to attend to — he has learnt to prioritise and the best ways to work with his teams.
“Patient care is the main reason why I chose to practise as a hospital clinical pharmacist. I feel rewarded when patients’ conditions improve,” he said.
While he has learned that some ideas may seem at odds with regular practice, the number of licensed collaborative pharmacists has shown that “healthcare practice can only advance with innovative ideas”.
Mr Lim has come a long way from the young town boy who loved biology and chemistry, and who chose pharmacy because he was able to get a study loan and not burden his parents. But he is still the filial son — and now also loving husband and father — who eats dinner with his parents and family every night. They do something for fun on weekends, and go on holiday every year or two.













 Get it on Google Play
Get it on Google Play