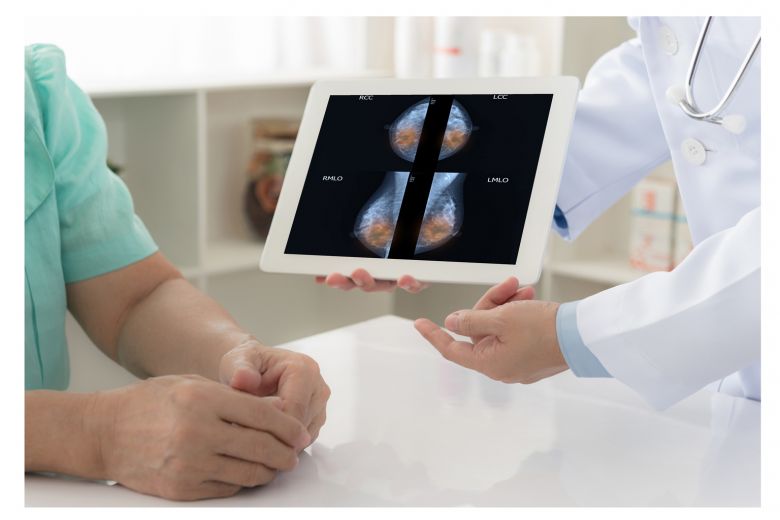
In the Impassion 130 study, triple-negative breast cancer patients treated with immunotherapy and chemotherapy survived 7.2 months without the disease progressing, compared with 5.5 months in the chemotherapy- only group. PHOTO: ISTOCKPHOTO
Global study shows immunotherapy, combined with chemotherapy, can help to extend lives of patients with aggressive breast cancer
News that combining chemotherapy with immunotherapy can help extend the lifespan of triple-negative breast cancer patients offers hope for those inflicted with this aggressive and hard-to-treat cancer.
It is a breakthrough for immunotherapy as breast cancer was thought to be unresponsive to the body's immune system.
Immunotherapy is a type of cancer treatment that enhances or makes it easier for the body's natural defenses to fight cancer.
The news follows a large-scale study involving 902 patients at 246 medical centres in 41 countries, of which eight patients were from Singapore.
The Impassion 130 study examined the effectiveness of the immunotherapy drug Atezolizumab, which belongs to a class of drugs called checkpoint inhibitors, in aggressive breast cancer.
Triple-negative breast cancer patients treated with immunotherapy and chemotherapy survived 7.2 months without the disease progressing, compared with 5.5 months in the chemotherapy-only group.
Triple-negative breast cancers are those that test negative for two hormone receptors as well as a cancer cell surface protein known as HER2. They therefore do not respond to endocrine therapy directed at hormonal receptors or targeted therapy directed at HER2.
The Impassion 130 results were more impressive for a subgroup, or about 40 per cent of these patients, who had PD-L1 positive tumours. Their overall median survival rate was 25 months on the combination therapy, compared with 15.5 months on chemotherapy alone.
"This is the first time we have seen survival results for the combination of chemotherapy with immunotherapy in triple-negative breast cancer and it is likely to have a meaningful impact on the way metastatic triple-negative breast cancer is treated in the future," said Associate Professor Rebecca Dent, head and senior consultant at the Division of Medical Oncology at National Cancer Centre Singapore (NCCS).
The lead author of the Impassion 130 study is Professor Peter Schmid, clinical director of London's St Bartholomew's Hospital's Breast Cancer Centre.
Prof Dent, who recruited patients for the Impassion 130 trial, was an invited speaker and attendee last week at the European Society for Medical Oncology (ESMO) 2018 Congress in Munich, where the findings were presented.
Dr Wong Seng Weng, consultant medical oncologist at The Cancer Centre in Singapore, who also attended the congress, said the study's results are "sufficiently robust to probably gain regulatory approval" from the United States' Food and Drug Administration, the European Medicines Agency and the Health Sciences Authority here for the use of immunotherapy in breast cancer and is, therefore, "a game changer".
Atezolizumab is not new and is approved for other cancers.
In Singapore, approximately 15 to 20 per cent of relapsed breast cancer patients every year are afflicted with triple-negative breast cancer.
"Triple-negative breast cancer is the most complicated type of breast cancer that we treat. Those with this form of cancer live about a year after their cancer comes back," said Prof Dent.
"It also affects younger patients. I had a 27-year-old patient with three kids and she lived just 12 months. It's devastating."
The median age of triple-negative breast cancer patients in Singapore is 55 years old, with the youngest at just 21 years old, according to NCCS.
At NCCS, Prof Dent has recruited two patients for an Impassion 132 study, which is also evaluating Atezolizumab.
Unlike the Impassion 130 study, which was for patients who relapsed more than a year after treatment for metastatic triple-negative breast cancer, Impassion 132 is for the early relapsing patients, or those who relapsed less than a year after adjuvant chemotherapy.
NCCS and the National University Hospital are two of the 83 centres that are recruiting patients for this worldwide study, and NCCS aims to recruit at least six patients or more if the enrolment is still open, said Prof Dent, who is the study's co-global lead.
Since the study opened in March this year, nearly 100 of the 350 patients worldwide intended for the trial have been enrolled.
As immunotherapy drugs are not cheap - they may cost $10,000 a month - more research is needed to figure out how long the patients need them for, as well as which other type of patients can benefit from it, said Prof Dent.
The two studies are not the only trials for those with triple-negative breast cancer at NCCS.
Globally, there are dozens of trials looking at the use of immunotherapy for different types of breast cancer patients, said Prof Dent.
Source: The Straits Times © Singapore Press Holdings Limited. Permission required for reproduction
Contributed by














 Get it on Google Play
Get it on Google Play