Early holistic treatment of chronic wounds could minimise the number of amputations in Singapore.
Early treatment of chronic wounds can make the difference between losing or saving a limb. Singapore’s major lower limb amputation rate is 28.5 per 100,000 population, which is much higher than all the Organisation for Economic Co-operation and Development (OECD) countries, based on data published in 2015.
It is estimated that currently one in 20 Singaporeans is afflicted with chronic wound conditions. This is expected to increase with Singapore’s ageing population and prevalence of diabetes. For better care for such patients, Changi General Hospital’s (CGH) Wound Healing Centre (WHC) provides multidisciplinary early intervention and outpatient treatment of chronic wounds. The team comprises wound specialists with background in orthopaedics, vascular, plastic, reconstructive and aesthetic surgery, as well as wound care nurses.
A wound that does not heal within four to six weeks is classified as a chronic wound. “People with such wounds are advised to seek medical attention early. Studies have shown that preventive interventions, early diagnosis, timely treatment and continued care benefit the healing of chronic wounds, and help reduce amputation rates and severity of amputation,” said Dr Derek Ho, Director of WHC, and Consultant, Department of Surgery (Vascular), CGH (pictured below).

On the other hand, delayed wound healing can put the patients at higher risk of complications such as infections and gangrene. In serious cases, one may even need to undergo an amputation. About 200 amputations are done in CGH yearly due to diabetes or peripheral vascular diseases.
As most chronic wounds are caused by multiple factors, the underlying cause may not be obvious without further investigation. A holistic multi-pronged approach therefore expedites the diagnosis and treatment process. The WHC is designed as a one-stop facility, where patients can undergo diagnostic tests, assessments and treatment all within the same day. This reduces the need for multiple visits to receive appropriate care.
Polyclinics, general practitioners, emergency departments and community hospitals can give patients a direct referral to the WHC and secure a consultation within two weeks. Currently, the centre provides an average of 1,000 wound-related consultations and procedures each month.

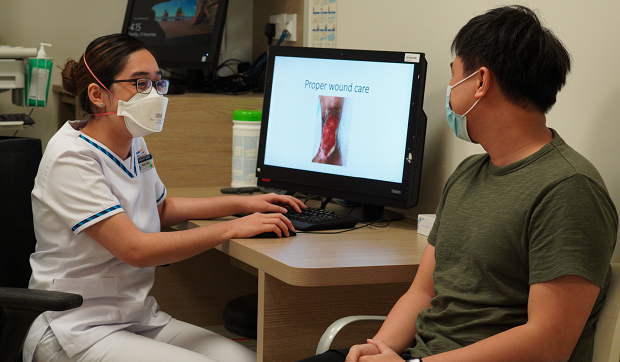
<<Dr Derek Ho and Senior Nurse Clinician Cheng Shu Hua carrying out followup assessment and treatment of a patient.>>
Global threat
Chronic wounds are an escalating problem worldwide. “Many countries are terming this as a silent epidemic because they affect a large fraction of population and numbers are expected to increase further,” said Ms Png Gek Kheng, Co-Director of WHC, and Chief Nurse, CGH (pictured below).

“Patients with chronic wounds have a reduction in quality of life due to the burden of wound care and associated complications. Most people have the perception that it takes time for wounds to heal, and some seniors think that poor healing is a normal sign of ageing. Smaller and hidden wounds may also be ignored by patients until they present with an infection. However, such wounds may deteriorate or become infected rapidly, and may lead to severe consequences,” she added.
Read more: Diabetes foot complications can lead to amputations. Click here to find out what to do and avoid.
Multi-pronged approach

<<Dr Kinjal Vidyut Mehta, Senior Consultant in CGH’s Orthopaedics Department, discusses a complex case with Dr Ho.>>
During the first consultation, the CGH care team will assess the wound and conduct tests, such as an ultrasound scan of the blood vessels to determine whether blood supply is obstructed. Based on the results from the diagnostic tests and the patient’s medical history, the wound specialist then recommends a treatment plan — be it for a diabetic foot, arterial or venous ulcer. Treatment is multidisciplinary. For example, CGH’s orthopaedic surgeons can look into corrective foot surgery for patients whose foot structure has been affected due to diabetic neuropathy. The condition affects the bones, joints and soft tissues of the foot or ankle, and causes an increased risk of pressure ulcers.
However, if the wound area is relatively huge with exposed bones, vessels or tendons, then the patient may need to undergo a reconstructive surgery by CGH plastic surgeons to close the wound. This is a procedure whereby the muscles, skin and blood vessels are transferred from one part of the patient’s body to another to cover the wound. These wounds can take up to three to six months to heal post-surgery.
During this period, patients who require a more intensive wound care regime will have to travel regularly to the WHC for wound dressing change.
Patients whose wounds are not significantly infected can be managed as an outpatient case at the WHC. This way, the centre also helps avoid or reduce the need for hospitalisation. In fact, some of the geriatric patients from WHC may be managed in the community by CGH community nurses as part of continued care. At the same time, CGH is also working with community hospitals and nursing homes to identify patients with chronic wound symptoms for referral to the WHC. In future, elderly patients who visit CGH’s Integrated Building for their outpatient appointments can also get a direct referral to WHC, if they have wounds at risk of becoming chronic.
“Having treated chronic wounds over the years, we understand the immense pain and emotional distress that these non-healing wounds can bring to patients and their caregivers. When such wounds are presented during the late stages, they become harder to treat and can take months or even years to heal. A holistic and coordinated care approach will shorten the runway for the healing process,” said Ms Png.

In the past, treatment for chronic wounds predominantly focused on the antimicrobial part of wound healing, where it was assumed that natural wound healing can occur by just clearing infections alone. However, medical professionals have learnt that this was not true, as there may be various underlying medical reasons why a wound is unable to heal properly.
Dr Derek Ho said, “Wound healing centres around the world are increasingly moving towards multidisciplinary treatment models. Over the years, wound treatment has expanded to include proper blood circulation, as good oxygenation and blood flow to the wound are needed for it to heal. The condition of the skin surrounding the wound, the patient’s overall health, nutrition, and the prevention of new wounds are also factors that are taken into consideration now.”
Get the latest updates about Singapore Health in your mailbox! Click here to subscribe.












