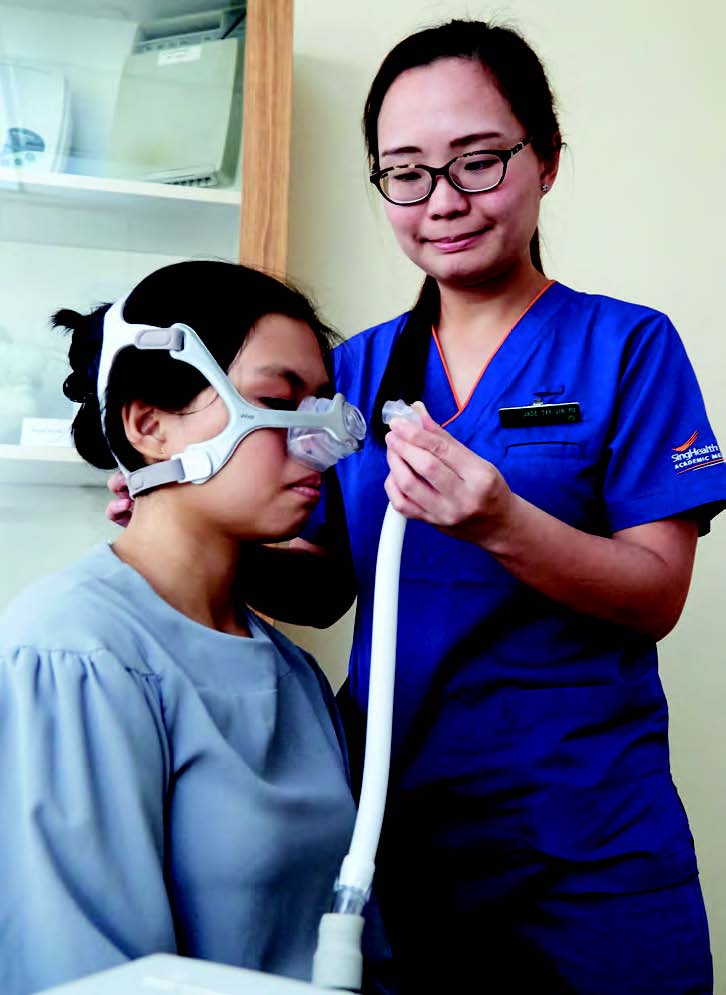
Photo: Vernon Wong
It’s most rewarding for this sleep technologist when her patients enjoy better quality of life because they can sleep well.
Sleep Technologist Ms Jade Tay truly understands what some of her patients go through.
Ms Tay works two nights every week as part of her job at Singapore General Hospital’s (SGH) Sleep Disorders Unit, putting her at risk of developing the kind of problems that her patients go through: poor or interrupted sleep.
While she does experience some of these issues, she employs some of the “tricks” that she teaches patients to help her adjust. Before the day of her night shift, she goes to bed later and wakes up later. She also tries to nap before going to work to get enough rest before pulling her 12-hour night shift. Working out at the gym also helps her sleep better.
“After working in this field for so many years, I’m used to it,” said Ms Tay.
Indeed, when she holidays in a different time zone, she doesn’t have much of a jet lag. “It just feels like a night shift.”
While some may shun shift work, especially long night ones, it was the night work and flexibility that drew Ms Tay to her job. Fresh out of school in 2013, Ms Tay, who graduated with a Diploma in Biotechnology from Temasek Polytechnic, saw the SGH ad, and the rest is history.
Working two 12-hour nights, then a sleep day, followed by two regular days allows her to spend time with her parents, with whom she lives. She has older married siblings.
At the time, she had little understanding of sleep disorders, but has grown passionate about the subject over the years. Today, she has learnt enough to train others — not just colleagues interested in the science, but also healthcare professionals from other countries in the region.
Into the night
The Sleep team, of which Ms Tay is a member, comprises psychologists, psychiatrists, neurologists, otorhinolaryngologists and respiratory specialists, as well as other sleep technologists. She conducts sleep studies or sleep tests that monitor patients while they sleep. The tests track the different stages of sleep that patients go through to determine if and why patients are not sleeping well.
“On the night shift, I have to set up the sleep test sensors — all 24 of them — on patients. I then check that they are working well before recording starts,” said Ms Tay.
During the night, she makes sure the sensors stay on and are working properly. She helps patients take them off if they need to use the toilet, and puts them on again after.
Although she would be alerted if something is amiss, she spends a good part of the night looking at a computer screen to make sure the test is going well. Two or three technologists work the night shift, which means they can take turns to rest. On her day shifts, Ms Tay analyses the sleep data collected and guides patients on using their devices correctly.
The most common conditions seen at the unit are sleep apnoea (interrupted breathing during sleep) and insomnia. For those with sleep apnoea, a device known as continuous positive airway pressure (CPAP) needs to be used during sleep. Ms Tay makes sure that patients get a well-fitting mask and that they understand how it is used.
Because of poor sleep, her patients tend to be short-tempered. But when they tell her they have had the best sleep in a long time following treatment — as did one patient — that is her best reward. “It means the treatment was effective,” Ms Tay said.













 Get it on Google Play
Get it on Google Play