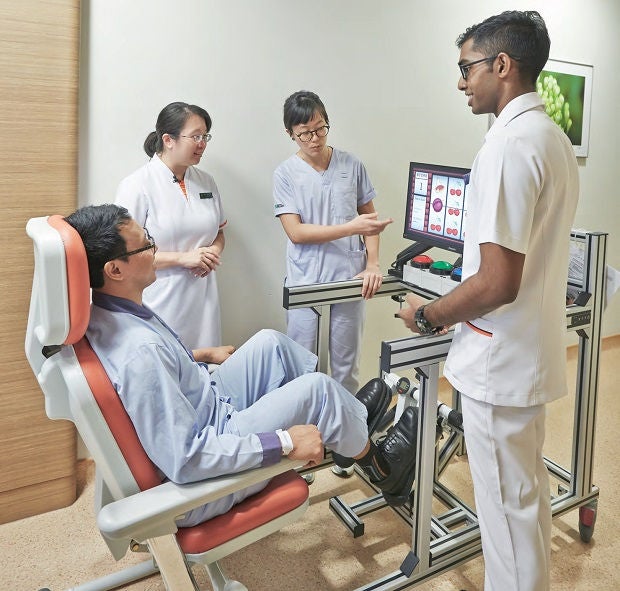
Designed to bring fun and convenience to inpatients, innovative healthcare applications initiated by nurses get tested by patients.
Araft of new devices and applications being piloted at Singapore General Hospital (SGH) promises to deliver more efficient care to patients while freeing nurses from routine and time-consuming tasks. Leveraging on digital technologies, the devices and applications will also help empower patients to be partners in their own health.
The pilot trials are expected to be implemented across other SingHealth institutions over time.
Hitting the jackpot
This fruit machine pays no money when the jackpot is struck. But when three identical images are aligned, the prize is far bigger.
It is a machine that a group of SGH nurses and physiotherapists devised to help inpatients avoid muscle weakening as a result of prolonged bed rest. Patients sit on a hospital chair and pedal away on the exercise stepper, which triggers the jackpot reels to start spinning. When the patient has pedalled enough times, the reels will show a winning line and — jackpot!
Another game in the same exercise system incorporates both exercise and memory training. When the patient stands up, one of the fruits lights up. Before the light goes off, the patient must press a coloured button corresponding to the colour of that fruit. At higher, more difficult levels of the game, two or three fruits light up.
The game motivates patients to not only stand and sit, but also strengthens their memory because they have to focus their attention on the fruit that lights up, said Ms Ang Shin Yuh, Deputy Director of Nursing Quality Research and Transformation, SGH.
With Singapore’s ageing population, hospitals are expected to face a greater number of increasingly older patients. “For an older patient, the risk of complications is higher. Even with one or two days of bed rest, their risk of muscle loss or deconditioning is higher. So we wanted to create an environment where they can recover faster, and can do rehabilitative exercises much quicker,” said Ms Ang.
Built with input from the engineering faculty of Singapore University of Technology and Design (SUTD), the system is being piloted at the SGH Internal Medicine Ward. The aim is to recruit 30 patients for the six-month trial.
Digital menus
It’s not quite the Ritz, but “room service” at some SGH wards just got a bit easier and quicker.
An application that is downloaded onto an iPad allows patients to ask for beverages, and additional pillows and blankets. That information is conveyed to the nurses, who can then act on the requests immediately. Patients no longer have to ring a bell and wait for a nurse to attend to them before they can put in their request.
More importantly, the MyCare app holds the patients’ individual medical and health information during their hospital stay — the tests and procedures they are scheduled for, their results, the readings of their vital signs, information on the medications they are taking, and other educational materials. Having such information lets patients better understand their treatment and recovery process, helping them to be more involved in their own care.
“The nurses started this to empower patients to take charge of their own care even after they’re discharged from hospital, with the hope of reducing readmissions,” said Ms Tan Sheng Lian, Assistant Nurse Clinician, SGH.
The app, which is password-protected, was developed by SingHealth nurses, doctors, allied health professionals, Office for Service Transformation, and IT specialists from the Integrated Health Information Systems.
The MyCare app started as a pilot at two SGH wards but will be rolled out at other SGH wards, as well as Changi General Hospital, KK Women’s and Children’s Hospital, and the National Heart Centre Singapore by 2021.
Continuous monitoring
Patients who have just had surgery need to have their vital signs — heart rate, respiratory rate, temperature, and blood pressure — monitored every couple of hours. As they also need their rest and sleep, it can be a bit of a bother when they are awakened every so often to get these signs measured.
Another innovation that nurses have developed is a wireless wearable biosensor that automatically and continuously monitors patients’ vital signs. The palm-sized, self-adhesive device, which is placed on the patient’s chest, also triggers real-time alerts should any of the vital signs go out of the normal range. This allows for a speedy response from the medical team.
The sensor is mostly used on patients who have had surgery or blood transfusions, or are newly transferred from the intensive care unit. The initial version of this application was piloted in November 2018. Trials on the updated version started in March 2019, and the second SGH ward in the test started its pilot in July 2019.
Ms Tan added that two other wearable monitoring devices are also being piloted.
One is the oxygen saturation monitoring clip, which is attached to the hand to continuously measure the patient’s oxygen saturation.
The other is a blood pressure cuff that checks the patient’s blood pressure at pre-set intervals. The patient is not awakened from his sleep, as is often the case now, when nurses need to check his blood pressure.













 Get it on Google Play
Get it on Google Play