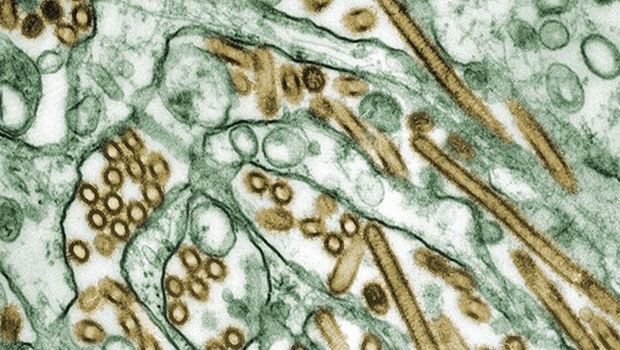
The current outbreak of a highly contagious strain of H5N1 avian influenza has been called the worst in history. By January 2023, poultry farmers in the US had slaughtered almost 60 million birds infected or at risk of being infected with H5N1, with a similar number being culled in Europe while in Japan, farmers set out to kill more than 10 million chickens.
It is not just poultry and wild birds that are being infected. In Peru, nearly 3,500 sea lions died from the virus. Cases have also been reported in otters, wild dogs and foxes.
But this strain of H5N1 is not new. It was first identified in 1996 in farmed geese in Southern China and Hong Kong, where the following year, it jumped from birds to humans, infecting eighteen people, killing six. Since then, variants of the virus have infected more than 800 people around the world, with 240 from Southeast Asia and China, the most recent cases hailing from Anhui Province in China and Cambodia, where an 11-year-old girl died from the virus.
So why are public health officials on high alert this time? Influenza expert Professor Gavin Smith, director of the Emerging Infectious Diseases Programme at Duke-NUS shares his insights.
H5N1 has been circulating for more than 20 years and there have been relatively few cases in humans. Why are public health officials keeping a close eye on this virus?
Smith: H5N1 has a very high fatality rate in humans, so it has consistently been considered a top pandemic threat. Since 1996, H5N1 has been commonly found in poultry across Asia. Because of live-bird markets—where people can buy a chicken or duck and have it freshly slaughtered—there is a huge exposure of people, both shoppers and workers, to the virus. This has resulted in sporadic infections, and some limited human to human transmission in the past. So there is concern that given enough chances the virus could adapt to efficient spread in humans.
The World Health Organization has said the risk to humans of this virus is low, but they are now reassessing. What’s changed?
Smith: In the last few years, H5 viruses (not just H5N1 but other N subtypes) had become more widely spread in wild birds and poultry across the world. The virus was initially restricted to Asia, then found its way to Europe and Africa before finally crossing to North America, first in 2014, which quickly died out by 2015, and then again in 2022. Subsequently H5N1 viruses have been detected in South America.
This wider geographic spread has increased the exposure of humans and other mammal species, such as seals, to H5N1 infection. This naturally increases the chances that the virus could adapt to mammals and potentially humans. While there is no evidence for this at the moment, it is important that the situation is closely monitored.
What do we know about the recent cases in Cambodia? Is there any evidence that the virus is passing between people?
Smith: There were only two confirmed cases in Cambodia, the daughter and father. There is no evidence that there was transmission between the pair, it could also have been from two independent infections from poultry.
Are you concerned that the virus may be evolving to spread more easily among humans?
Smith: At this stage, no. There is no evidence for adaptation to efficient human transmission. But repeated infection of mammal species, including humans, always increases that risk.
Some experts say that the strains that have been spreading since 2020 may be causing less lethal illnesses in people. Is that true, and if so, what would that mean in terms of assessing the pandemic risk of this virus?
Smith: This is very hard to assess, and I am personally not convinced either way. We are not even sure of the extent of human infection in many countries because surveillance is either not done or is insufficient. Regardless, even if the virus was less deadly than in the past, it would still cause a pandemic similar in severity to SARS-CoV-2.
The WHO has called for wider production of H5N1 flu vaccines. What other steps should countries be taking to prevent a possible outbreak?
Smith: We need to develop smarter ways of controlling the virus in animals, primarily through vaccination. Vaccination in poultry won’t prevent infection by H5N1 but it does reduce the overall amount of virus in the poultry population, which leads to less spillover into humans. This approach has been successfully used in many countries to prevent human infection. Because people mainly get infected from poultry, we should concentrate on reducing the amount of virus in live-bird markets and farms.
For instances when a spillover event spirals into a sustained outbreak, what can we do to have vaccines ready fast enough to avoid costly lockdowns?
Smith: The development and testing of universal influenza A vaccines—that would protect against most known influenza subtypes (the H and N combinations)—has been ongoing for many years. Since the COVID-19 pandemic and the success of mRNA vaccines, work has also started on mRNA vaccines that would protect against both influenza A and B. If these efforts are successful, we would be in a position to rapidly roll out vaccination in the event of an influenza pandemic.
The FDA has just approved the first OTC home-based flu test, could that offer us an edge in surveillance of suspected human cases?
Smith: Because this test kit does not distinguish between types of influenza A viruses, it would not be of much use.
Obviously, in a world still coming out of the COVID-19 pandemic, people are going to be very anxious about what might be next. Overall, how worried do you think people should be about this virus?
Smith: We have been studying these viruses for more than 25 years, and we have vaccines for birds available and human vaccines have been tested. There is also a good track record of influenza vaccines being used in people and we also have influenza specific anti-viral medicines. So overall, we are in a better position than when SARS-CoV-2 emerged. COVID-19 has also left us better prepared. We are more vigilant and already taking steps to prepare for a possible pandemic.












