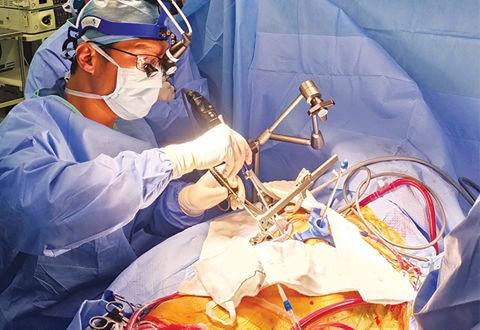
Asst Prof Chua Kim Chai performing a minimally invasive cardiac surgery.
Heart valve disease is the leading cause of cardiovascular morbidity and mortality globally1. Common valve diseases include stenosis (valve narrows and does not open properly) of the aortic valve and the mitral valve, and tricuspid valve regurgitation (valve becomes ‘leaky’ and does not close properly). When one or more valves do not work properly, blood flow is affected and this will put extra strain on the heart and make it work harder.
Advances in treatments for heart valve disease
Most patients with heart valve issues typically have one or more damaged heart valves which can be managed with medication to alleviate the symptoms, or surgery to repair or replace the valves.
Traditionally, an open-heart surgery is the only option to repair or replace the damaged heart valves, which requires a long recovery period. In the last decade, advanced valve therapies such as the Transcatheter Aortic Valve Implantation (TAVI) and MitraClip, have increasingly become more common and mature in technique, offering a lifeline to patients who are at high risk for conventional surgery.
First of its kind procedure
More recently, NHCS performed its first minimally invasive double valve repair procedure, an endoscopic-assisted double valve surgery where both damaged heart valves are corrected in one procedure.
“NHCS has been providing minimally invasive valve repair and replacement via thoracotomy (small incisions) on the side of the chest between the ribs for suitable patients, as the benefits are evident including minimising the need for blood transfusion during operation, faster recovery and shorter hospital stay,” said Asst Prof Chua Kim Chai, Senior Consultant, Department of Cardiothoracic Surgery.

An illustration of how a right mini thoracotomy is done, with a thin video camera inserted through a small incision.
A case study: Minimally invasive double valve repair
81-year-old Mdm Ong suffered from severe heart valve disease for decades. She had mitral stenosis and tricuspid regurgitation, and had multiple hospital admissions for heart failure symptoms such as shortness of breath and an overload of fluid in her body arising from her heart condition. Mdm Ong had declined surgery due to considerable risks associated with an open-heart surgery. However, over time, her symptoms worsened and she could not walk more than a few steps without stopping to rest.
Despite her advanced age and the severity of both heart valves, Mdm Ong had no other major health issues. Judging from the severity of her heart condition, an open-heart surgery would have been the only option to improve her health and quality of life. However, given her age, the risks in open-heart surgery would be greater including longer recovery time, potential wound complications and lingering breathlessness.
Upon further assessment of Mdm Ong’s health condition, a mini thoracotomy mitral and tricuspid surgery was recommended.
During the surgery, small incisions were made in the side of the chest and long instruments were inserted into the incisions to reach the damaged valves. Asst Prof Chua successfully replaced her mitral valve, which was too thick and stiff to function properly, with an artificial valve, and repaired her leaky tricuspid valve by tightening the ring (annulus) around the valve using a medical device.
Now, with advancements in minimally invasive surgery allowing both of her damaged valves to be corrected in one procedure, Mdm Ong is back on her feet faster than expected and walking without feeling breathless.
In contrast to traditional surgeries, which offer an unobstructed view of the surgical field, Asst Prof Chua shares, “Performing minimally invasive procedures can pose challenges, and their success relies on careful pre-operative planning. In the case of a double valve surgery, the surgeon must enter both the left and right heart atria instead of just one, as well as have mastery of the technique to impede blood flow into the atrium to gain a good visual of the valve.”
Who is suitable for a minimally invasive double valve procedure?
Generally, minimally invasive (double) valve procedure is beneficial to most suitable patients as it is less invasive and offers faster recovery. However, Asst Prof Chua shared that there are exceptions, such as individuals who have had previous chest wall surgery, and those with high lung artery pressure or very poor heart function. He added, “Patients are advised to go for thorough assessment by doctors to determine an appropriate treatment option to achieve the best outcome. Those who lead an active lifestyle or are expected to have delayed chest bone healing from an open-heart surgery, are expected to benefit the most from minimally invasive procedures.”
MINIMALLY INVASIVE VALVE PROCEDURES IN NHCS | |
|---|---|
| There have been significant advancements in advanced valve therapies such as in the techniques and devices used, leading to improved outcomes. Increasingly, NHCS is seeing more patients being aware of the benefits of less invasive techniques which has considerably lower risks compared to conventional surgery. Other minimally invasive valve therapies that NHCS offers include: | |
ENDOSCOPIC-ASSISTED procedures where a fibrescope with lens at one end and video camera at the other allows the surgeon to view and operate the inside of the body:
| CATHETER-BASED procedures where a thin tube called a catheter, carrying a small device, is inserted into a blood vessel, and guided to the area requiring repair/replacement: |
Reference: Valvular heart disease epidemiology: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9228968/Update. American College of Cardiology Expert Analysis. 21 March 2019.
This article is from Murmurs Issue 46. Click here to read other articles or issues.












