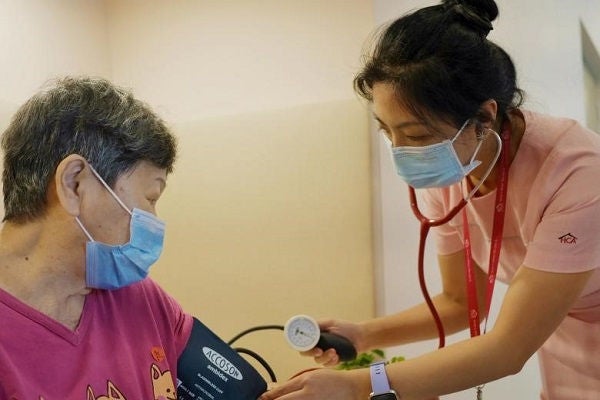
A member of HCA Hospice Care's home palliative care team visiting a patient at her home. PHOTO: HCA HOSPICE CARE
By the time palliative care is offered to a patient in an acute hospital here, he will most probably die within the fortnight.
Such support services need to be offered sooner, experts said, particularly as a majority of people would rather die at home.
A 2020 Singapore Hospice Council (SHC) survey found that more caregivers whose loved ones had died at home felt they had died in their preferred place of care, as compared to caregivers whose loved ones had died in the hospital, said Dr Shirlyn Neo, chair of the caregiver survey subcommittee.
Feedback was collected between September and October 2020 from 143 caregivers whose relatives had recently died.
The SHC aims to advance public understanding on hospice and palliative care, support efforts to improve service quality and provide training.
The quality improvement workgroup within the SHC also studied the quality of care and service planning for the financial years from 2017 to 2020.
About 12,000 referrals to palliative care were made on average each year for 9,000 patients.
The study found that the interval from when a patient was referred to his or her death was 12 days on average for those in acute hospitals, 18 days for those in inpatient hospice care, 44 days for those under home or day care services, and 95 for those in outpatient clinic care.
"The data means that we are reaching patients very late in the illness journey," said Dr Grace Yang, senior consultant at the department of supportive and palliative care at the National Cancer Centre Singapore.
It shows there are opportunities to extend help sooner to patients, she added, calling for palliative care capacity to be expanded, particularly in the community.
At a palliative care conference in December, Health Minister Ong Ye Kung said the Government is boosting capacity for day hospice and home palliative care places.
Experts like Dr Yang have noted a measurable difference when palliative care is extended to patients and their families early.
A Lien Foundation survey on death attitudes conducted in 2014 found that over three-fourths of Singaporeans prefer to die at home. Yet public data shows that in 2020, only a quarter of deaths occurred at home, she noted.
In comparison, SHC's minimum data set found that among those referred to hospice home care - which is usually earlier than other types of palliative care - around 50 to 60 per cent were able to die at home. "This suggests that hospice home care services render support to patients and families so that they are more likely to be able to fulfil their wish of passing away at home, if that is their preferred place of death," said Dr Yang.
She suggested working with primary care providers in hospitals and the community so that patients who are well, living at home, and still receiving disease-directed treatment can also receive palliative care aimed at relieving symptoms and stress of serious illness.
Beating the taboo of discussing death
More also needs to be done to cut through the taboo of talking about death.
People sometimes associate palliative care professionals with "angels or harbingers of death", said those in the industry.
HCA Hospice Care receives almost 300 referrals a month from hospitals, clinics and others. A proportion of these cases reject its service. "They will say 'Who asked you to call me? My father doesn't know he has cancer, don't come and visit us'," said HCA's medical director Chong Poh Heng.
Just half of Singaporeans are open to discussing end-of-life plans with loved ones, a Singapore Management University study last year of some 5,200 Singaporeans across different age groups found.
A majority of respondents said they thought more about the end-of-life stage compared to other life stages amid the pandemic. Yet only 53 per cent of them said they would plan for this, compared to 97 per cent for marriage and 93 per cent for having children.
"This will go down as the most taboo project I have ever undertaken," said senior statistics lecturer Rosie Ching, who led the study that was done in collaboration with Direct Funeral Services. "I personally experienced rejections from many quarters, many bordering on hostility."
Mr Gabriel Lim, a programme director with the Lien Foundation, said it can be hard to address a taboo so deeply entrenched in Asian culture. "Using a medium such as the arts can be a good way, where people don't have to confront the topic head on but still be engaged," he said.
The Lien Foundation has worked with partners on various outreach efforts such as a video series, graphic novel and getai campaign on the topic of death and dying.
A role model may be provided by Taiwan, said Mr Lim. It is the highest ranked Asian society on the Quality of Death Index in 2015, commissioned by the Lien Foundation. Taiwan ranked sixth while Singapore came in 12th.
Taiwan organisations rope in people like hairstylists and taxi drivers to become community advocates while death education, termed "Life Education", is part of mainstream curriculum for students in Primary 5 to high school.
In Singapore, the My Legacy portal was launched for beta-testing in 2020 as a public resource for end-of-life matters.
A Public Service Division spokesman said it offers services and resources on end-of-life planning, as well as where to find palliative care, home care support and caregiver support.
The portal offers a secure vault function to store important documents securely online and share them with loved ones through Singpass log-in.
As at December last year, the portal has about 120,000 users, of which 5,522 are registered vault users, said the spokesman.












