Radiology has advanced far beyond x-ray imaging to become an important component of life-saving treatments.
Technological advances allow today’s radiology department to go beyond using x-rays for both diagnosis and therapy.

<< X-rays were introduced in hospitals in 1913.>>
Within three years of its discovery by Wilhelm Roentgen in 1895, the first x-ray apparatus was installed in Singapore. X-rays were more a curiosity than a diagnostic test then, and it was only in 1913 that x-ray services were introduced in Singapore General Hospital (SGH).
Since then, SGH has been at the forefront of some of the most important radiology-related developments in the region. In 1983, SGH was the first public hospital to acquire a computed tomography (CT) scanner, where a computer reconstructs x-ray images taken into two- and three-dimensional (2D and 3D) images.This led to dramatically improved diagnostic accuracy, and marks a quantum leap in radiology practice.
Radiology has gone beyond just using x-rays for diagnosis. Ultrasound and magnetic resonance imaging (MRI), which do not use x-rays, are safer and offer different perspectives of “looking inside” the human body.
Technological advances have led to a phenomenal range and sophistication in radiological imaging, which means more accurate diagnoses and prognoses, and better care and treatment.
Today’s scanners not only allow us to “see” our internal anatomy and disease process clearly and in fine detail, some can also evaluate physiological functions and biochemical constitutions of internal organs and tumours. Magnetic resonance spectroscopy differentiates between types of brain tumours, while perfusion imaging assesses the adequacy of blood supply to the heart or brain in a heart attack or stroke.
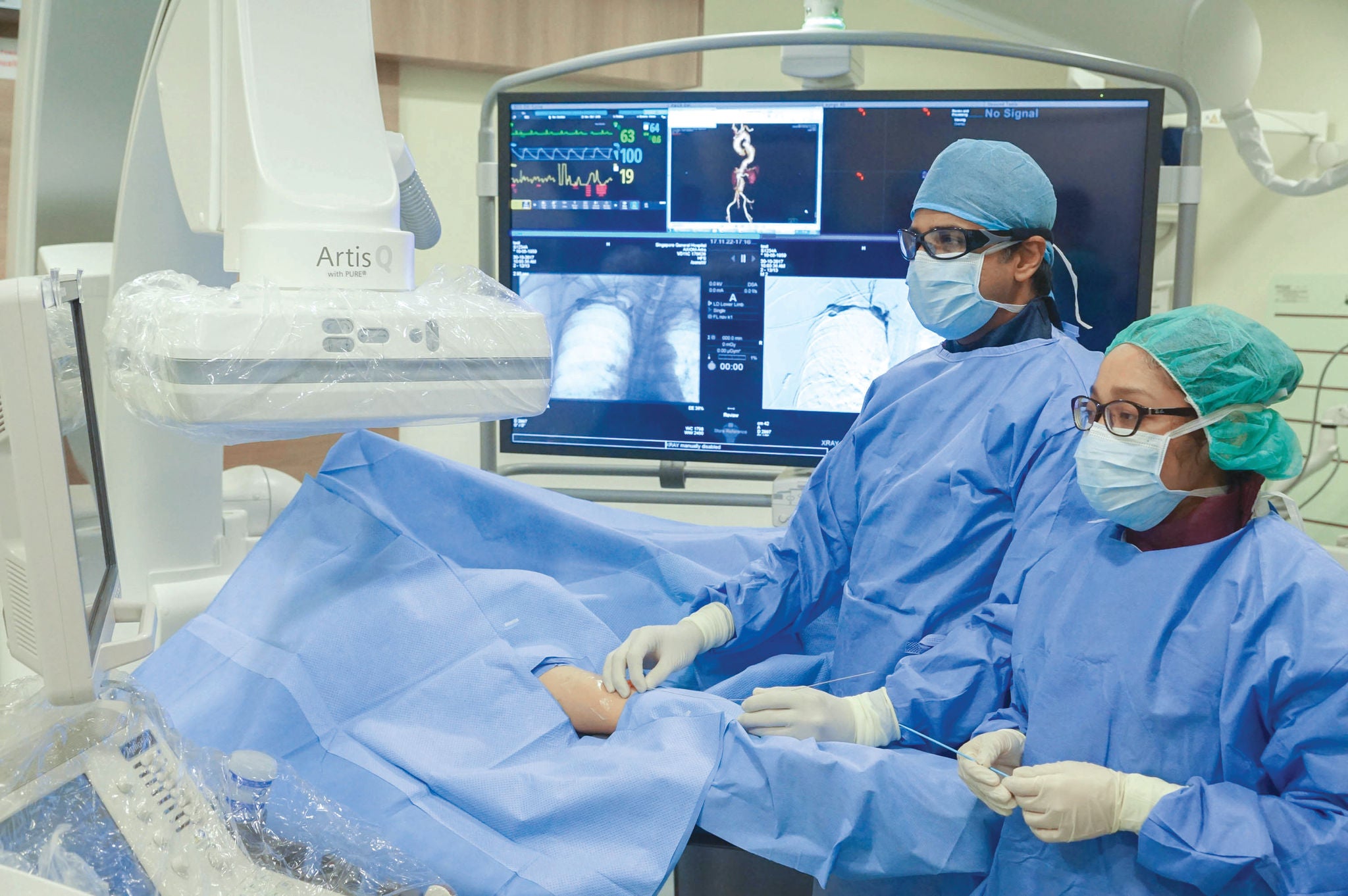
Significantly, radiology has stepped firmly into the realm of therapy, offering minimally invasive treatments with the help of imaging guidance. Interventional radiologists, for one, are specialists whose work has blurred the divide between imaging and treatment.
Angiography, introduced in the 1950s, marks the beginnings of interventional radiology (IR). With x-ray guidance, imaging of blood vessels is performed by direct needle puncture. With better imaging guidance, refinements in catheters and guidewires, and miniaturisation of medical devices, IR experienced exponential growth from the 1980s.
An indispensable service in hospitals, IR sees more procedures being performed for treatment, rather than for diagnosis, today. At SGH, nearly 12,000 IR procedures are done each year, from routine to emergency limb- and life-saving treatments.
Together with surgery,chemotherapy and radiotherapy, IR is the fourth pillar of cancer therapy. Interventional radiologists use scans to accurately locate tumours, then insert a needle into the organ to burn or freeze the tumours. They can also administer anti-cancer drugs or radioactive substances into the blood vessels.
Established in 1980, the Department of Nuclear Medicine remains Singapore’s only stand-alone nuclear medicine department. A top nuclear medicine centre in the region, the department has strengths in areas that surpass centres in the US and Europe. In 2003, Singapore’s first cyclotron was installed in SGH in a joint venture to produce positron emission tomography (PET) radionuclides for use in nuclear medicine.
Nuclear medicine uses radioactive-labelled drugs or materials for cancer, cardiac, and neurological imaging. During the imaging scans, small amounts of a radioactive substance (radiotracers or radiopharmaceuticals) are injected or introduced into the body. Radiation emitted from radiotracers bound to molecular characteristics specific to the tumour, helps localise tumours with high precision, image various body systems, and decide on management. Similarly, in radionuclide treatment, radiotracers are injected to target cancer cells, sparing the healthy ones.
In 2017, SGH’s radiology-related services were consolidated into the Division of Radiological Sciences for streamlining and collaboration of diagnosis and image-guided therapy. The division includes the Departments of Diagnostic Radiology, Nuclear Medicine and Molecular Imaging, Radiography, and Vascular and Interventional Radiology.













 Get it on Google Play
Get it on Google Play