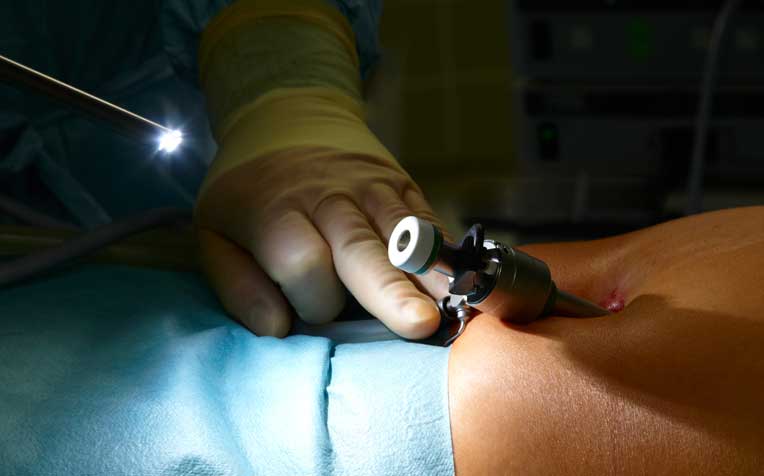
Obstructive jaundice can be treated with keyhole surgery.
Dr Tan Ek Khoon, Associate Consultant, Department of Hepato-pancreato-biliary and Transplant Surgery, Singapore General Hospital (SGH), a member of the SingHealth group explains the signs and symptoms as well as treatment options for obstructive jaundice.
Signs of obstructive jaundice
Watch out for yellowing of the skin and the whites of the eyes, which may be followed by itching of the skin. As the condition worsens, other symptoms may appear:
- Severe abdominal pain
- Fever
- Chills
- Vomiting and nausea
Treatment of obstructive jaundice
Depending on the underlying cause, the doctor may initially prescribe pain medications and antibiotics to treat the infection if the cause is related to gallstone disease. Diagnostic imaging and blood tests will usually be able to distinguish the various causes of jaundice. Definitive treatment will depend on the cause of the jaundice.
If gallstones are diagnosed, endoscopic removal of the stones obstructing the bile duct is recommended. Endoscopic stenting is sometimes necessary as a temporary measure to relieve the bile duct obstruction and clear any bacterial infection before definitive surgery. Thereafter, laparoscopic (keyhole surgery) cholecystectomy is advised to remove the gallbladder, from which most gallstones originate from.
If the root cause of obstructive jaundice is a malignant tumour, the long-term outcome of such patients is best served if the tumour can be surgically removed.
Such surgery is a major undertaking and patients should be managed by hepato-pancreato-biliary surgeons (surgeons specialising in liver, pancreas and biliary problems). The outcomes of such major surgeries are also better when they are performed in a high-volume and dedicated surgical centre.
Unfortunately, the majority of patients with malignant tumours may not be suitable for surgery, hence, chemotherapy and/or radiotherapy will be the next best option. For such patients, the obstructive jaundice can be relieved through the insertion of a stent by endoscopic guidance or radiologic guidance, once the diagnosis of cancer is established.
“If obstructive jaundice is left untreated, there is a high risk of infection when bilirubin overflows into the bloodstream. More importantly, it is vital to distinguish the various causes of obstructive jaundice. Painful obstructive jaundice is often associated with gallstone disease. Painless obstructive jaundice is associated with tumours but patients generally feel fine and seek attention late, leading to delays in treatment,” says Dr Tan.
To prevent jaundice resulting from gallstone disease, eat a healthy, balanced diet and reduce your intake of fatty foods and alcohol.
Ref: P16
Conditions & Treatments
Public Events
Get the Health Buddy App
© 2025 SingHealth Group. All Rights Reserved.













 Get it on Google Play
Get it on Google Play