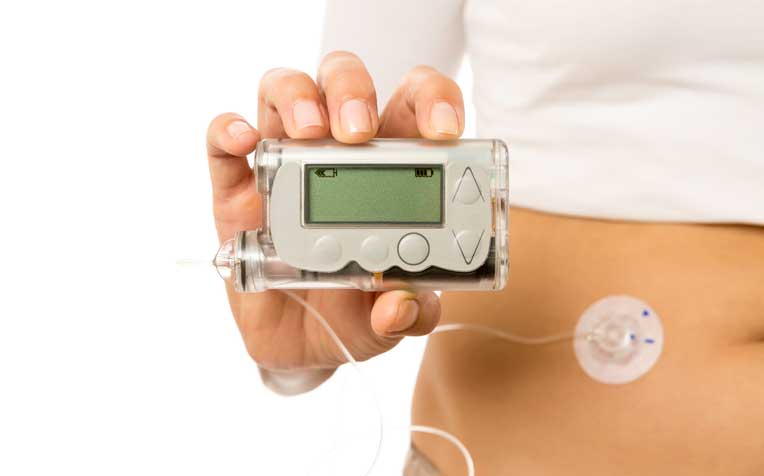
Insulin pump therapy is a good option for people who have poor control over their diabetes.
A palm-sized pump which administers insulin to diabetics via an infusion set can help reduce episodes of low blood glucose level
Mr Wong Leng Hoe, a diabetes patient and user, dubbed it the “portable pancreas”. Worn discreetly on the body, the palm-sized, pager-like insulin pump delivers the hormone round the clock. It mimics closely the normal discharge of insulin by the pancreas to regulate the body’s glucose or sugar level. Insulin is needed to convert carbohydrates into energy, and without it, sugar builds up in the blood, which can lead to serious health problems.
Mr Wong, who switched from injections to using the insulin pump in July 2013, carries the device with him 24/7. “I used to forget to inject the insulin – or not do it altogether – when it was inconvenient to do so, like when I was having lunch with clients.
“With the pump, I don’t have to excuse myself to go to a quiet place to prepare the insulin and inject myself. I merely press a button to deliver the (higher) dose of insulin needed before a meal. And I don’t have embarrassing blue-black marks on my body because of the injections,” he said.
Diabetics need to adjust the amount of insulin they use before meals or sports, as their blood sugar levels can go up (after a meal) or down (when exercising).
Mr Wong, who is in his 50s, was diagnosed with type 2 diabetes more than 15 years ago. This form of the disease, also known as adult-onset diabetes, is associated with obesity and an unhealthy lifestyle, unlike type 1 diabetes where the pancreas isn’t able to produce insulin. Type 1 diabetes is an autoimmune disease and is often diagnosed in childhood.
Type 1 diabetics require insulin treatment from the onset of the disease, while treatment for type 2 involves medication, or insulin injections when the disease progresses and medication is not enough to control the disease. Type 2 diabetes develops when the body becomes resistant to insulin or when the pancreas stops producing enough insulin to control the amount of sugar in the blood.
Insulin pump therapy: a good option for those struggling to control their diabetes
According to Dr Bee Yong Mong, Senior Consultant at the Department of Endocrinology, Singapore General Hospital(SGH), a member of the SingHealth group, insulin pump therapy is a good option for people who have poor control over their diabetes. Mr Wong, for instance, struggled to control his diabetes even after starting insulin therapy more than 10 years ago.
“Over the years, we’ve had to increase his insulin dosage significantly,” said Dr Bee, who is also Director of the Diabetes Centre, SGH.
With the pump, “fast- or rapid-acting insulin is delivered via an infusion set which includes a short, soft tube, called a cannula, that sits comfortably under the skin of the abdomen,” said Dr Bee. The device pumps out insulin in a steady, measured and continuous dose 24 hours a day (this is known as the basal rate), and is also capable of discharging a surge of the hormone when needed (this is known as the bolus dose).
Before a meal, a patient decides how much more insulin he needs based on his blood sugar reading, and presses a button on the pump to push extra insulin units into his body. The extra insulin is needed to account for the carbohydrates consumed, and to bring the patient’s glucose levels back to a specified target range.
After a month on the pump, Mr Wong’s diabetes was better controlled. He no longer saw large swings in his blood glucose levels, and he could be more flexible about what and when to eat.
Studies elsewhere have shown that patients on insulin pump treatment can achieve better diabetes control and reduce the incidence of hypoglycaemia, a condition where the blood sugar levels are abnormally low, Dr Bee said. When hypoglycaemia occurs, diabetics can lose consciousness if they don’t eat something sweet quickly to raise their glucose levels.
Insulin pumps have been in use in Singapore for more than 20 years, but few patients opt for it, mostly because of the cost. The pump is expensive and is not covered by local medical insurance, unlike in the US for instance.
Prices range from $2,500 to $9,000 for a pump, and consumables like the infusion sets will set the patient back by another $150 to $200 a month. The infusion set, which includes the cannula, needs to be changed every three days.
“In the US, 50 per cent of type 1 patients are on pump treatment, as they can claim the costs from their insurance. In Singapore, the adoption rate is low,” Dr Bee said, noting that only about six patients at SGH – mostly type 1 diabetics – use the pump.
Mr Wong paid about $2,700 for his – a mid-range model – but he is just glad that he now needs less insulin than when he was on injections.
Diabetes affects about 10 per cent of Singapore’s population, with the type 2 form of the disease accounting for 90 to 95 per cent of sufferers.
One-week training before patients start on insulin pump treatment
Patients who opt for the insulin pump treatment are trained for a week by a team comprising a doctor, a dietitian, a diabetes nurse and a representative from the insulin pump supplier. “We will work with the patient to get him acquainted with the equipment, his diet and to improve his knowledge of the insulin pump. The doctor will then decide on the amount of insulin that he should use,” said Dr Bee.
New location, more facilities
The refurbished Diabetes Centre in Singapore General Hospital (SGH), which relocated to its new location at SGH Block 1 Basement 1 in June 2013, has more consultation rooms. It also has a facility for staff to create fundus photographs that show clear pictures of the retina and other parts of the inside of the eye.
Diabetes patients can lose their sight if diabetic retinopathy, a complication of the disease, is not detected. The disease has few symptoms until it is at an advanced stage. By then, the patient may have limited or no vision.
At the centre, patients can now have their retina tested and their results ready before they see their doctors.
Said Dr Bee: “The patient comes to us, we take a picture of his retina and the image is sent to SAILOR (Singapore Advanced Imaging Laboratory for Ocular Research). The report comes back to us quite quickly and we can see the patient on the same day. This frees up the doctors’ time and improves the care of patients too.”
In the past, doctors like Dr Bee had to interpret the results, which took time. But now the images are transmitted instantly to SAILOR – part of the Singapore Eye Research Institute (SERI) – for interpretation by accredited technicians.
Since July 2013, the technicians have examined the retina images of 163 SGH patients, of which 47 were referred to the Singapore National Eye Centre (SNEC), said Ms Haslina Hamzah, Programme Manager, SAILOR. Of the patients referred to SNEC, a member of the SingHealth group, 25 were found to be suffering from diabetic retinopathy.
She said that about 30 per cent of diabetes patients in Singapore have diabetic retinopathy, with 10 per cent having a severe form of the disease.
Ref: R14
Contributed by

















