Continuous glucose monitoring systems provide a more complete picture of glucose trends and patterns.
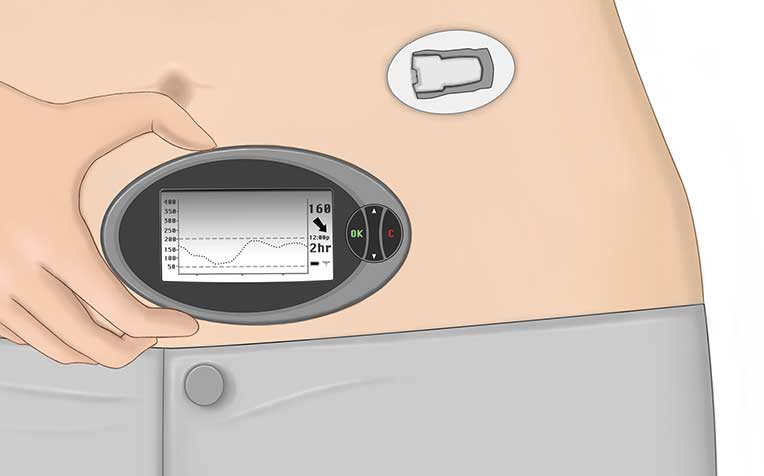
Continuous glucose monitoring systems are devices that include a sensor, a transmitter and a receiver (Figure 1).

A continuous glucose monitoring system samples interstitial glucose levels every few minutes, which allows for collation of all the glucose values into glucose curves (Figure 2).

Each sensor is able to provide readings typically for up to 6 days. This helps to fill in the gaps of missing information from doing only intermittent capillary blood glucose readings (Figure 3a).
"Continuous glucose monitoring systems enable a more complete picture of glucose trends and patterns to enable more precise insulin dose titration," says Dr Daphne Su-Lyn Gardner, Senior Consultant from the Department of Endocrinology, Singapore General Hospital (SGH), a member of the SingHealth group.
As a continuous glucose monitoring system samples glucose readings every few minutes rather than snapshots of the capillary glucose at any one point of time (Figure 3a), it is able to provide information on the glucose trajectory (Figure 3b). This allows the user and healthcare provider to overcome what would have been ‘blind spots’ in the glucose profile.

Figure 3a: Self-monitoring of capillary glucose readings (mmol/L) over the course of 5 days

Figure 3b: Continuous glucose monitoring tracing over 1 day. With continuous glucose monitoring, glucose curves are generated that allow a more comprehensive view of glucose trajectories beyond capillary glucose readings, and how food/medication/exercise interact with glucose levels.
Continuous glucose monitoring may either be retrospective for diagnostic purposes or it may be used in real-time.
Diagnostic continuous glucose monitoring systems are blinded to the individual who is wearing it. It is used by the healthcare professional to:
- Detect asymptomatic or nocturnal hypoglycaemia, and
- Aid in titration of medications, insulin doses or nutritional adjustments.
Real-time continuous glucose monitoring also contains alarms which can alert the user if the glucose level is rising or going below a pre-set threshold. This will allow the user to make changes to prevent or correct a high or low glucose level.
Most real-time continuous glucose monitoring requires once to twice daily blood glucose calibrations (involving fingerprick glucose tests) and each sensor lasts for up to 6 days.
"Real-time continuous glucose monitoring has been shown to improve overall glucose control in terms of improvements in HbA1c and reduction of the frequency of hypoglycaemia, particularly in those with type 1 diabetes," says Dr Gardner.
However, real-time continuous glucose monitoring needs to be used regularly for this improvement to be effected.
In addition, real-time continuous glucose monitoring may be combined with insulin pump therapy to allow for automated insulin suspension in response to, or prior to, a pre-set low glucose level. It may also be used in the future to control the high glucose levels by automatically controlling delivery of basal insulin.
Ref: D21
Contributed by

















