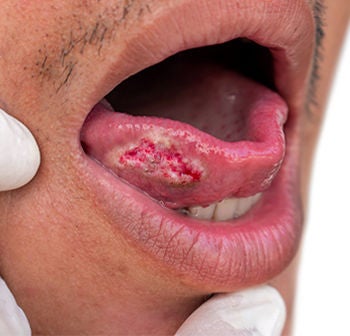
A symptom of tongue cancer includes ulcers in the mouth that do not heal, even after two weeks.
Although tongue cancer is not among the top ten cancers in Singapore, in recent years, National Cancer Centre Singapore (NCCS) has recorded a three to fourfold increase in tongue cancer cases among women aged 35 to 55.
When 35-year-old Karen (not her real name) discovered an ulcer on her tongue, she consulted her family doctor.
When it did not heal, she had it checked at a hospital, where they did a biopsy and told her she had nothing to worry about. But she had an uneasy feeling as the lesion was growing, although there was no pain.
She researched it, then consulted a specialist at NCCS.
Professor Gopal Iyer, Head and Senior Consultant, Division of Surgery & Surgical Oncology at National Cancer Centre Singapore, a member of the SingHealth, group, examined it and was worried even though the biopsy was negative.
“I suggested surgery to remove it. I reasoned that if I was wrong she’d lose just a bit of her tongue. But if I was right, I’d have saved her from tongue cancer,” Prof Gopal Iyer said. Karen agreed.
“I removed a quarter of her tongue. She recovered well and went home two days after the operation. A week later, the results confirmed that the lesion was indeed cancerous,” he said.
Karen was lucky to have caught it early. Her persistence, in the absence of obvious symptoms, paid off.
Symptoms of tongue concer
Symptoms of tongue cancer include
- Ulcers in the mouth that do not heal,
- White or red patches in the mouth that cannot be scraped off,
- Lumps on the tongue,
- Swelling in the mouth and
- Pain when chewing or swallowing food
Ulcers that commonly come about when you accidentally bite your lip or tongue when chewing or talking should resolve within one to two weeks.
However, if the ulcer lasts more than two weeks, has irregular edges or hard nodules, or is growing quickly, it may be worrying.
Another way to differentiate between the common ulcer and one you should be worried about is the absence of pain.
Most non-cancerous ulcers are painful due to inflammation. However, cancerous ulcers may not be painful at the beginning, making them more suspicious.
But not all tongue cancers start with an ulcer. Some notice a lump on the side of the neck that grows over time and becomes painful.

Tongue cancer: an evolving incidence
Previously, most sufferers were men, with the ratio being three male cases to one female. Now, the incidence is equal between the genders.
This trend is seen in other developed countries, but what is puzzling doctors here is that these female patients do not have the same triggers as before.
In the past, a typical tongue cancer patient was an elderly man who had been smoking and drinking his whole life. Smoking is a known cause of tongue cancer, along with sexually transmitted diseases (STDs) such as the human papillomavirus (HPV).
Today’s female patients do not have HPV or other STDs. They do not smoke, drink, or chew betel nut or tobacco. Nor are they associated with recently suspected causes – poor dentition (sharp teeth or badly fitted dentures) or the long-term consumption of immunosuppressants following treatment for kidney cancer, leukaemia or lymphoma.
NCCS’ clinician scientists embarked on a complex study to get to the bottom of the mystery.
Principal investigator Prof Gopal said they have ruled out HPV as a cause.
“In tongue cancer, the first thing we look for is HPV, but their tests proved negative. I confirmed this finding with a group in the United States engaged in a similar study. We also looked for genes the tumour might express, but there weren’t any clear-cut answers.”
Undeterred, they moved on to genome sequencing − at press time they had sequenced 18 samples, and were decoding the tumour’s genetic information and analysing the data they had collected.
“Some promising genetic markers have come up, and we’re trying to validate this. If we find specific genes such as enzymes causing the cancer, and if they can be targeted, that will be very promising. It’ll not just tell us what’s causing the cancer, but open up the possibility of creating an inhibiting drug,” said Dr Gopal.
Two theories
Definitive answers have not yet been found, but Dr Gopal has learnt enough to propose two theories.
Firstly, many women with tongue cancer may already have a higher genetic risk of the disease. This risk, combined with a previous short but sustained exposure to cigarettes (whether by smoking or inhaling second hand smoke), may kickstart the cancer.
Secondly, there is a suspected (though unconfirmed) link with diet. According to Dr Gopal, these young women with a higher genetic risk of tongue cancer may have also been eating processed foods and cooked food with carcinogens.
Besides this, he also cited a study showing a link between the overuse of alcohol-based mouthwash and tongue cancer.
Treatment for tongue cancer
Treatment typically involves surgery to remove the cancer, radiation therapy and chemotherapy and/or targeted drug therapy if the cancer is found to be at an advanced stage.
If detected early, only a small portion of the tongue needs to be removed.
But if the cancer is more advanced, a larger portion of the tongue will need to be removed, thus affecting the patient’s speech and ability to swallow. In such cases, the doctor may recommend reconstruction of the tongue, along with radiotherapy and chemotherapy.
Early-stage tongue cancer, has a reasonably high five-year survival rate of 70 to 80 per cent, but falls to 50 per cent for the intermediate to advanced stages.
As early detection is your best protection, should you discover a lump, no matter how small it is on your body, do get it checked by a doctor as soon as possible.
Ref: G25 (ed)

















